Subscribe if you want to be notified of new blog posts. You will receive an email confirming your subscription.
Search Results: "Medical home"

Medicare MAPCP Medical Home Demo: CMS Kicks Sands in the States’ Faces
by Jaan Sidorov, MD and Vince Kuraitis
The Medicare MAPCP (Multi-Payer Advanced Primary Care Practice) demo promised to be Medicare’s Biggest Change in 40 Years…
…but the emerging reality isn’t living up to the promise.
In this post, we’ll discuss:
The Promise
An Overview of the MAPCP Demo
Our Main Takeaway: Emerging Reality Suggests Medicare Will Be a “Difficult” Partner
Conclusion: Think Twice Before Signing Up
1) The Promise
The sandbox metaphor was first used by the National Academy for State Health Policy:
For the 10 or more […]

Three Years Of Medical Home Demonstration Preparation Down the Drain?
Do you remember the scene in the movie Animal House where Bluto Blutarski laments “…seven years of college education down the drain?”
Why aren’t primary care physicians expressing similar laments about the shelving of the MMHD (Medicare Medical Home Demonstration) in favor of the MAPCI (Multi-Payer Advanced Primary Care Initiative).
My colleague Jaan Sidorov, MD and I pick up on no signs of discontent. Read our essay “Three Years of Medical Home Demonstration Preparation Down the Drain?” on Dr. Sidorov’s blog.

CMS Shelves Medicare Medical Home Demonstration
I just received an email from CMS announcing the latest official word on the Medicare Medical Home Demonstration (MMHD):
10/26/2009 – In Washington, the efforts to reform health care and health insurance include proposed legislative language that would have an impact on the Medicare Medical Home Demonstration as described in section 204 of the Tax Relief and Health Care Act of 2006 and amended by section 133 of the Medicare Improvements for Patients and Providers Act of 2008. Specifically, section 1302 of […]

Part II — The Medicare Medical Home Demonstration: Crawling Out From Under the Rock
In Part I of my guest post on The Collaborative Forum blog, I wrote that the Medicare Medical Home Demo is in BIG Trouble. Here’s a recap:
Political reality dictates that the MMHD must save costs.
As currently structured, the MMHD cannot achieve cost savings
In any given year, only a small percentage of patients account for the vast majority of costs
Lessons from previous Medicare disease/care management demonstrations has shown that effective care coordination interventions must be targeted at this population
Medicare has structured the […]

Medical Home Savings Claims in Medicaid are Not Plausible
by Al Lewis, Disease Management Purchasing Consortium International, Inc.
Medical homes probably do save money in very controlled settings, where the entire team is literally or at least figuratively under one roof, such as Kaiser. However, the belief that one can overlay a traditional medical home model across an entire state and save money in the process turns out to be total fiction.
The poster child for that fiction, North Carolina’s Community Care program, turns out to cost state taxpayers probably $400 […]

Medicare Medical Home Demo (MMHD) is in BIG Trouble
Between the time the MMHD was authorized in 2006 and now, we’ve learned a lot about what works and what doesn’t work in Medicare care coordination programs. The MMHD is between a rock and a hard place — conflicted by two “must achieve” objectives that are diametrically opposed:
As a political matter, the MMHD must save money
As currently structured, the MMHD cannot save money
Please read my guest post
The Medicare Medical Home Demonstration (MMHD): Between a Rock and a Hard Place
over at […]
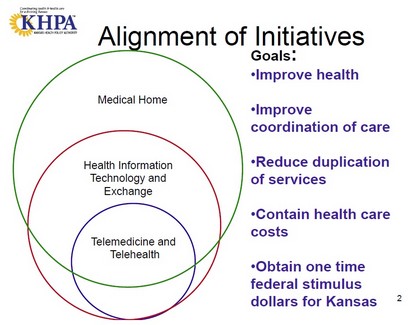
HITECH Overlap: Medical Home, Telehealth, Health IT/Exchange
What’s the commonality among Medical Home, Telehealth, and Health IT/Information Exchange initiatives?
They all relate to care coordination. As shown in the diagram below from the Kansas Health Policy Authority (KHPA), there’s a lot of overlap.
A larger copy of the slide is available in this March 2 PowerPoint presentation by Marcia Neilsen , Executive Director, KHPA.
What are some of the implications?

Medical Home “Model” Transmogrifies to: The Medical Home Movement
Part Medical Home 101, part strategy session to rescue primary care, part revival meeting — the National Medical Home Summit held earlier this week in Philadelphia was an amazing event.
The optimism, energy, and dogged persistence of attendees and presenters was pervasive. The event was standing room only with another 200 people tuning in to a live Internet video cast.
Dr. Joseph Scherger captured the mood of the day when he proclaimed:
The Medical Home “model” has […]

Complimentary Issue — Medical Home News
Would you like to receive a complimentary issue of a new publication — Medical Home News ? Click on the link and then on “Sample Issue” in the upper left corner.
Here’s a preview of the first issue:
Introducing Medical Home News
An Annotated Guide to the Medicare Medical Home Demonstration (MMHD)
Subscriber’s Corner
Johns Hopkins Lipitz Center to Assist Practices in Medical Home Demo
National Medical Home Summit to be Held March 2nd – 3rd 2009
Thought Leader’s Corner
Industry News
Catching Up With… Paul Grundy, MD
I’m honored […]

JAMA Article Asks: What About “The Other Medical Home”?
Dr. Steven H. Landers writes a thoughtful article in today’s JAMA . He asks why the term Medical Home doesn’t include the patient’s home:
“…the Medical Home initiative, as currently articulated, ironically fails to emphasize the complex chronically ill patient’s actual home. This represents a failure to recognize the profile of the highest-risk beneficiaries driving much of the high Medicare costs—that is those with or more chronic conditions and activity limitations…
“A promising way to strengthen and broaden the Medical Home initiative […]