Subscribe if you want to be notified of new blog posts. You will receive an email confirming your subscription.
Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs
Google Health (GH) could be the event of the decade in advancing health care reform — not just healthcare information technology (HIT) reform, but health care system reform. GH promises simultaneously to create AND dominate the market for next generation personal health records (PHRs). There is nothing else in our solar system or in the entire universe like it.
While Google has not “officially” announced the details of GH, they’ve left a lot of clues. In this essay I’m going to play a combination of detective and tea leaf reader — deciphering existing clues and making some educated guesses about where GH is headed….it’s very exciting.
I get truly inspired when I see a business model that 1) is exceptionally powerful, and 2) offers dramatic benefits to humanity. Google Health is just such an animal.
Let me be clear. I am not speaking for Google; I don’t work for Google. This posting is my collection of inferences drawn from the clues provided about GH and from my general knowledge of health care and business. So when I write “GH will ______”, recognize that this is me putting together clues and applying my best judgment.
Here’s an overview:
- The Current Market Structure for Personal Health Information (PHI)
- GH’s Anticipated Technology Model
- Three Leverage Points
- GH Will Be Disruptive
- Concluding Thoughts
One last note before we dive in — this is a long blog posting and some of it will require careful attention to grasp the full picture.
I. The Current Market Structure for Personal Health Information (PHI)
The situation is sad, but not difficult to describe. Your health care and wellness information is 1) scattered everywhere, and 2) not in standardized formats suitable for a global information economy.
First, PHI is scattered. From a patient’s POV: “Information about my health and health care is scattered everywhere. Most of it is on paper, while some might be electronically stored. This information exists in the records of doctors, hospitals, pharmacies, labs, imaging centers, therapy centers, counselors, etc. Some of it is still in my head.”
The physician’s perspective is a mirror image of the view of an individual patient: “Information about all my patients’ health and health care is scattered everywhere….
Here’s how Adam Bosworth, VP, Google and head of GH, described the problem:
There is no place individuals can go to get a comprehensive set of health and medical information about themselves. Access to this comprehensive information can be vital to proper and timely diagnosis of the patient, to the patient getting the best possible treatment, and, perhaps sometimes overlooked, to the patient getting the best possible ongoing care and support after the initial treatment, especially for chronic illnesses. [Bosworth; December 7, 2006]
Second, not only is information scattered, but standards for defining and sharing the data are still evolving; where standards exist, many of them predate the Internet. Standards about how to define consistently the information (clinical standards) and to transmit and exchange the information (technical standards) are not yet formalized and agreed upon:
Despite all these initiatives [CCHIT, HL7, IHE, ASTM, EHRVA, HITSP ] there exists no overall plan for how standards should be defined and the overall principles that should guide their design to ensure an optimal societal use of ICT [information and communication technologies]. Equally important, no one has identified all the standards needed to support interoperability of health care ICT. [National Bureau of Economic Research, May 2007]
II. GH’s Anticipated Technology Model
We’ve been provided a number of clues about the technology model that GH is likely to develop:
- Patient centric
- A personal health URL
- Automated data mechanisms to gather and store PHI
- Interoperable technical standards: XML and the Continuity of Care Record (CCR) standard
- A user interface
- Appropriate security and confidentiality measures
- Value added functionality (over time)
Let’s examine the clues one at a time.
a) Patient centric
Let’s put the patients in charge of their health and medical information. Let’s build a system which puts the people who are sick in control. For every single medical and health-related event, let’s make sure that patients can effortlessly retrieve and share their information in its totality and then use it to ensure that they get the best quality of care possible. It is their health. [Bosworth; December 7, 2006]
This vision for the future of health care starts with the premise that consumers should own their own total personal health and wellness data (I’ll call it PHW for short) and that only consumers, not insurers, not government, not employers, and not even doctors, but only consumers, should have complete control over how it is used. [Bosworth; May 22, 2007]
b) A personal health URL
The personal health URL and the supporting infrastructure is the cornerstone of the GH offering.
…every ill person needs a “health URL,” an online meeting place where their caregivers — with express permission from the ill person — can come together, pass on notes to each other, review each other’s notes, look at the medical data, and suggest courses of action. This isn’t rocket science. It is online web applications 101. [Bosworth; December 7, 2006]
c) Automated data mechanisms to gather and store PHI
The people who treat, diagnose, test or dispense medications to patients should be required to deliver, instantly, over the net, at the speed of light, that information to those patients to use as they see fit. If these patients choose to share it with caregivers or health coaches or nursing services, that should be their right. [Bosworth; December 7, 2006]
…the labs you take and the prescriptions you fill out and even the images of your body are usually not available to you in electronic form even though they flow through the net speeding their way to insurers and Pharmacy Benefit Managers (PBMs) and formularies so that, in the end, people can get paid. We believe that consumers have the right to demand that if this information is flowing, it should also flow to them. [Bosworth; May 22, 2007
After attending one of Bosworth’s speeches, consultant and blogger David Williams suggested that GH will negotiate with a range of parties (presumably health plans, labs, imaging centers, pharmacies, PBMs) to allow PHI to flow freely and appropriately:
Google wants to include in their PHR transaction data between physicians and health plans, physicians and PBMs, labs and physicians and so on. They are not planning to rely on feeds from physician EHRs to do this –Bosworth made a point of pegging EHR adoption outside the hospital at <10% though I think he’s understating the truth– but to try to plug directly into the payment streams.” [David Williams, World Health Care Blog]
GH has been fairly clear about its intent — the patient owns the data and has the right to access their own PHI. While there are few specifics, Google likely will use a combination of carrots and sticks to encourage and cajole various parties to help PHI flow freely into and from Google’s repository that feeds the patient’s personal health URL.
d) Interoperable technical standards: XML and the Continuity of Care (CCR) standard.
GH will employ XML to make personal health information transferable across different information systems.
…we have spoken to leading health providers and institutions from coast to coast, we have heard people say that it is too hard to build consistent standards and to define interoperable ways to move the information. It is not! Ten years ago, I heard people saying the same things about how hard it would be to build consistent standards for allowing programs all across the world to share data. I set out with a small band of people to build a standard way to share any information, XML. [Bosworth; December 7, 2006]
GH will embed the Continuity of Care Record (CCR) standard into its offering.
With the advent of standards such as the Continuity of Care Record (CCR) and Continuity of Care Document (CCD) to follow shortly, we are almost there when it comes to computable health data. … as Google looks at these standards and we will, undoubtedly, over time want to support both so that we can help search intelligently for phenotypic information and connect people with the information, places, people, and online expertise that they need, we are likely to endorse these standards, but with the caveat that we will all need precise encodings and precise dosages or quantities to be spelled out. So this is practically a reality. [Bosworth; May 22, 2007]
e) A user interface. Google will need to present users (patients, physicians, others) with an interface to access their PHI through their GH personal health URL. Google is known for starting with basic functionality and adding capabilities over time. Google has a number of options to develop a user interface: 1) GH could build its own user interface, 2) GH could acquire an existing PHR/EHR company and adopt its interface, and/or 3) GH might develop a crude user interface of its own, and allow existing PHR/EHR companies to compete to provide more sophisticated user interfaces to patients.
f) Appropriate security and confidentiality measures. While the devil is in the details, GH seems to appreciate that it must keep PHI secure and confidential. I understand that this issue by itself stirs a tremendous amount of emotion and debate, so I’ll simply acknowledge the importance of the topic without delving into the rat’s nest of inevitable details.
g) Value added functionality. Bosworth’s speeches and writings have hinted at a wide range of possible options:
- Patient information indicating progress compared to evidence based guidelines
- Drug interaction alerts
- Medically reliable (certified) health information
- Recommendations for health care providers fitting patient specific criteria
- Physician/hospital quality information
- Health coaching
- Decision support
- etc., etc.
Many of these and other options could be added over time; Google could choose to develop these additional modules on their own and/or encourage 3rd parties to develop plug-ins to GH.
III. Three Leverage Points
Before you can fully grok the potential of GH, you first need to understand three conceptual building blocks for GH:
- GH can simultaneously create AND dominate the market for next generation PHRs.
- GH can overcome the Achilles heel of current PHRs — the “populating the PHR” challenge
- GH’s business model can create a network effect and could result in rapid, accelerating adoption
A. GH can simultaneously create AND dominate the market for next generation PHRs.
Since 99% of the world would probably struggle with even a definition of a first generation PHR, let’s start there. According to Stephen Downs, SM, senior program officer and deputy director of RWJF’s Health Group:
The current understanding of a PHR is of an online repository of all of the information in your medical record—and that’s way too limiting. [A New Vision for Personal Health Records, RWJF Project HealthDesign; May 2007]
There are two categories of first generation PHRs, each of which has significant limitations:
1) Stand-alone PHRs. These PHRs typically require patients to gather and input their own data. Only a small percentage of patients are motivated or interested in gathering together their PHI, which you’ll remember is 1) scattered everywhere, and 2) not in suitable, standardized formats.
2) Tethered PHRs. Tethered PHRs have a sponsor— typically a health plan, employer, or delivery system. One advantage is that the sponsor often brings “some” data to populate the PHR — perhaps EHR data in the case of a delivery system or claims data in the case of a health plan. However, this data typically is neither interoperable nor transportable — the data will not transfer across multiple providers, and the patient typically cannot “take” the PHR with them when they leave a sponsor.
Tethered PHRs also have other challenges. Adoption is stifled because patients do not always trust that a sponsor is acting in the patient’s best interests. Finally, data that a sponsor brings usually is not complete and/or comprehensive; for example, health plans primarily have access to claims data, which is a proxy for clinical data, but certainly not a substitute.
What’s a “next generation” PHR? Think of first generation PHRs as an application — a end in and of itself, a “place” to store and access PHI. Think of next generation PHRs as BOTH an application and a platform. As a platform, the PHR is not just a place to store and access PHI, but it also becomes a means to support a wide range of new applications.
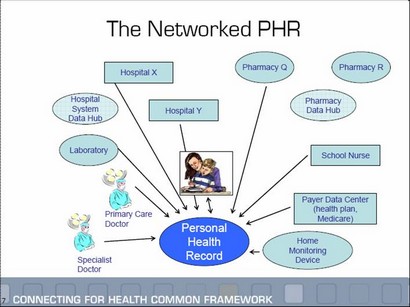
Indeed, the power of a personal health record lies in its potential to be coupled with alerts, reminders and other decision-support tools that help people take action to improve their health or manage their conditions. From this perspective, the personal health record can be seen as part of a broader personal health record system. Health care and technology pioneers are beginning to develop solutions that harness the power of PHRs to create consumer-friendly tools people can use in their daily life to stay healthy and better manage illness. [Overview—Personal Health Records, RWJF Project Health Design]
The Markle Foundation has also written eloquently about the evolution of PHRs. Their concept of the “Networked PHR” is shown in the diagram below. Feel free to substitute “Google Health” for the words “Personal Health Record”.
While there are 200 PHRs currently in the marketplace, there will be nothing else like GH.
B. GH can overcome the Achilles heel of current PHRs — the “populating the PHR” challenge
Recall that the basic problem with PHI is that it is 1) scattered everywhere, 2) not in suitable, standardized formats. One of the biggest challenges of current PHRs is simply getting your PHI into the PHR in the first place and then keeping the data current.
GH will create systems and standards to address the “populating the PHR” challenge.
1) GH will develop automated data mechanisms to gather and store PHI
As described in the section above explaining GH’s technology model, GH will work with various parties to help PHI flow freely and appropriately into and from Google’s repository feeding a patient’s personal health URL.
2) GH will make the CCR standard the “MP3” of Personal Health Information
While explaining the elegance and the simplicity of the CCR standard is beyond this essay, you will need to grok the CCR standard to really understand the potential of the GH offering. Think of the CCR as 80% of the value of an electronic health record achieved with 10% of the effort.
David C. Kibbe, MD, MBA, — who is acknowledged as one of the developers of the CCR standard — analogizes the CCR standard to the MP3 audio format.
Let’s set one thing straight — the MP3 is an inferior audio format:
- It doesn’t contain all the information of an original recording. Audiophiles sneer at MP3s because much of the high highs and low lows are lost by compressing the audio file.
- Not everything is available in MP3 format.
- It is not a universal format — not every device can play MP3s.
Despite these inferiorities, the MP3 is “good enough” to have taken the world by storm. According to TechWeb:
By the end of the 1990s, music fans discovered that a CD song title converted to MP3 would still sound pretty good even though it was only 1/10th the size of the original CD track. Smaller files meant faster downloading. At an average of 4MB, it took less than 15 minutes to download a file over an analog modem. With a broadband connection on a college campus, it took seconds.
Similarly, the CCR standard is an inferior PHI format:
- It won’t contain all your medical history
- It won’t contain all the detail even about the medical history it does provide
- It’s not a universal solution to broader HIT standards issues
But it’s good enough. The CCR standard:
- Provides a constantly updated record of important PHI
- Is mobile (movable)
- Is accessible through a wide range of devices and media
C. GH’s business model will create a network effect and can result in rapid, accelerating adoption
The author of the Theory of Disruptive Innovation — Professor Clay Christensen — notes that technology by itself does not create disruption. It’s necessary to have the right business model to create disruptive effects.
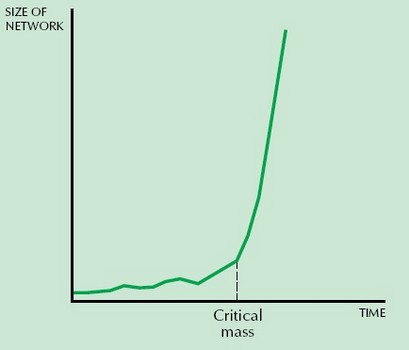
The GH offering promises to create a powerful network effect. As shown in the diagram below, a network effect in a market results in the value of the network growing exponentially based on the number of users.
NETWORK EFFECT
The classic example of a network effect is fax machines. When one person has a fax machine, the network has no value; when two people have fax machines, the network has “some” value because the two users can send faxes to one another. When the market reaches critical mass (the tipping point), network effects take over; adoption increases rapidly as people without fax machines feel compelled to join the network or be left out.
GH has potential to reach a tipping point rapidly: patients, government and employers will be openly enthusiastic about GH and will promote adoption (see the discussion below about disruptive potential).
The lack of suitable, formalized HIT standards creates an opportunity GH to set de facto standards. “A de facto standard is a technical or other standard that is so dominant that everybody seems to follow it like an authorized standard.” One example of a de facto standard is the Microsoft Windows operating system, which runs on about 90% of the world’s PCs,.
The timing for GH to set de facto standards around the use of the CCR standard is ideal. While the CCR standard is not yet widely used, the heavy lifting of creating and establishing it has been accomplished. The CCR standard has been approved by key standards bodies and has 11 sponsoring organizations, including HIMSS, the American Academy of Family Physicians, the American Academy of Pediatrics, the American Medical Association, and others.
Is Google powerful and influential enough to set de facto standards in health care? If not Google, who else could even try?
A business model with a strong network effect and defacto standards setting is necessary to solve the fundamental problems of PHI being 1) scattered everywhere, and 2) not in suitable, standardized formats. GH will place the data in one location (the patient’s personal health URL) and will present PHI in a suitable, standardized format (PHI that is updated through automated mechanisms using the CCR standard).
GH also likely will employ other tactics aimed at creating high barriers to entry
- free pricing to consumers
- patents
- economies of scale
- Using first mover advantage to create customer lock-in and switching costs
GH will build on build on Google’s existing capabilities — superior search technology, a strong brand, a proven revenue model, partnerships, and market leverage.
While there will be many opportunities to create revenue, Google’s existing primary revenue model (selling ads) undoubtedly will be a key aspect of GH. What’s not clear is how far Google can take PHI to created personalized and targeted ads. GH’s revenue model also cannot easily be duplicated by competitors whose core business is not Internet search.
IV. Disruptive Potential
GH will be very disruptive to existing economic interests. Here’s a quick first take how the GH might impact various players:
Patients/consumers – tremendous upside if Google can get past concerns about security and privacy.
Employers – significant upside. They will see GH as an important step toward HIT interoperability, transparency, greater consumer involvement in decision making.
Physicians – mostly positive, but GH could be confusing for doctors to understand.
- Can GH get past traditional physician caution to encourage rapid adoption?
- Can GH get physicians’ attention long enough to change their workflow? National physician organizations could take a leadership role here.
- GH is synergistic with the medical home model being promoted by primary care physicians. GH creates an opportunity for primary care physicians to reestablish a prominent role in delivering and coordinating care.
Health Plans – mixed.
- GH challenges proprietary IT. Many health plans are vested in their proprietary IT systems; they see proprietary IT as a source of competitive advantage. GH will promote interoperable exchange of information, and thus will challenge many health plans current thinking.
- GH challenges health plans “navigator” strategy. Many health plans are executing a strategy to position themselves as navigator of the health care system on behalf of patients. While this is a good strategy, it’s undermined by GH making the health system more navigable by consumers themselves with or without help from their doctor.
- GH turbocharges health plan cost containment and quality initiatives. The economic benefits of increased penetration of HIT accrue mostly to payers, not providers; the Markle Foundation estimated 89% of economic benefits go to payers. GH promises to be a catalyst for broader HIT adoption, which should make plans jump for joy.
- Bottom line: payers will have second thoughts (mostly privately), but will quickly recognize that resistance is futile and that GH provides many cost and quality benefits.
Hospitals – major disruption, but they will be unable to notice or react.
- Hospitals are a major target of cost containment efforts. Reducing admissions, ER visits and procedures is a major target of health care cost containment strategies.
- However, how does a hospital ever know about an admission that was avoided due to appropriate flow of patient health information?
Imaging centers, labs – mostly disruptive.
- Duplicative testing costs payers, even though it benefits imaging centers and labs
- However, the increased flow of electronic data promises some cost efficiencies over paper, fax, and phone.
V. Concluding Thoughts
Let’s go back to the beginning. The basic problem is that your PHI is 1) scattered everywhere, and 2) not in suitable, standardized formats. The GH technology model and business model offer solutions to both of these problems.
I find the prospect of GH very compelling. Patient care will improve. Costs will go down.
I hope that my projections about Google Health are only the start of a longer conversation. I look forward to your comments.
This work is licensed under a Creative Commons Attribution-Share Alike 3.0 Unported License. Feel free to republish this post with attribution.
[…] Vince Kuraitis at e-CareManagement.com has an excellent piece on Google’s foray into the healthcare world. Here’s the bait. (Google Health) GH […]
Wow! This is brilliantly explained and analyzed. But… didn’t Healtheon have a similar vision and approach? What they encountered was the disconnection between “payment centric information flow” or claims information and “clinically relevant information flow” or what is currently charted in paper format in the medical care transaction. How will Google create sufficient critical mass to drive individual physicians to document clinical care in a PHR environment? Alternatively how will Google incent physician offices to electronically connect to the network? In short, what will be the value proposition of the PHR/Google model to those that create 85% of the PHI – the individual practicianer? And as a correlate, what will be the value proposition be to the doc to convert from paper to electronic documentation of the clinical encounter? Today, payment structures drive documentation requirements and approaches. Can the Google model drive payment reform? If not, perhaps they, too will go the way of Jim Clark, never to tread into healthcare again.
Vince,
Terrific piece and thanks for the mentions of Project HealthDesign. In the discussion of next generation PHRs, we’re thinking of an architecture that has three levels: 1) the data typically held by a provider or other health care institution (i.e. your medical record); 2) the collection of these data, as well other user generated data (i.e. what you expect Google or other intermediaries to do); and then 3) the applications or tools that are developed to help people act on their data to improve their health. In my mind, each of these ought to have open (secure, of course) interfaces so that as a user, you can ask your provider to send your data to the service that you use to store your data (perhaps Google, perhaps others) and then, ideally, there’s a marketplace of developers building applications that both draw on the data your service holds and populate that service with data generated outside the care system (e.g. a pain diary, data on meds taken). I’ve fleshed out some of these ideas more on the Pioneering Ideas blog.
Definitely an interesting and well thought out article. However I do have, along with numerous others I suspect, serious concerns about Google maintaining my health information.
In a month where Google has been termed “hostile” to privacy (http://news.bbc.co.uk/2/hi/technology/6740075.stm), it is a huge leap to expect users to trust the company to fairly and honestly maintain their intensly private information.
The most significant barrier to useful PHR’s is not technological, nor is it centred around employeers concerns. Patient trust is vital and I would go as far as to suggest that companies perceived to be untrustworthy risk reducing the uptake of electronic health records rather than further this vital revolution in healthcare.
Well done – a really good analysis. Thank you.
Some points to consider: Do you exist in an information silo? Can you get out? Simon put it very well…personally i find it bizarre to think patients will entrust Google.
What if your Doctor has a problem with Google and will not use its service. Such problems can arise from unfair competition, fear of American big business culture or just plain old “they don’t pay me enough”.
Medical records aren’t the answer to everything and there are widespread misunderstandings from tech people of their value or a patients ability to create/manage a useful one. The consumer orientation of the google health record will mean it is so padded out that it will ineffectively consume vast amounts of individual physician time and it will be hard to find an acceptable way to reimburse for this.
Vince,
Congrats on a very timely and well thought out posting. It will be very interesting to see if a Google PHR will experience any greater consumer adoption that have health plan sponsored PHRs –
Continued Post
It will also be interesting to see how health plans in particular will respond if at all. After all this will not be the first time we have seen high tech companies (Healtheon, WebMD and Revolution Health) take a “veni, vedi, vici” approach to healthcare…only to have them die a slow death “trying to cross the Alps” – an allusion to the healthcare industry.
Like all new things in today’s evolving consumer/retail healthcare industry, it will be the consumer and not the pundits like me who will eventually decide how successful Google’s strategy will be. I wonder if Google brought any elephants along for the journey?
Physical Therapists utilize SOAP notes to track a patient’s progress.
These sheets have list space for subjective information (patient states greater pain after walking 30 mins yesterday), objective (patient able to perform 10 additional quad reps at level 2), assessment (patient progressing toward goals but not completely satisfied with speed of recovery – revise goals), and protocol (exercise program revisions, etc.).
Perhaps the ‘best’ or most useful PHR/EHR structure will not be a single EHR stored on a removeable memory stick (although wouldn’t that be handy???), but rather a combination of approaches dogpiled together using web-based applications.
This would allow the partnership of patients and caregivers in ensuring accuracy and utility of personal health as well as official medical record data, and the added bonus is that patients who are just not interested in being very involved can still leave the bulk of the work up to the medical professionals.
For example, using the SOAP analogy, I envision the subjective being a memory stick, CD-Rom, or Personal Health URL (or any/all of the above), ‘owned’ by the patient and accessible at the docs office/hospital.
The objective portion would be an EMR that nurses, docs etc. would pull up on laptops, or small flatscreens on moveable trays, stored within the hospital system/server but ‘reviewable’ by the patient either with a special access code, with an email address to the MR staff or the docs office/AA to contact if they see or suspect a mistake.
Likewise, patients could download information from their own hospital EM record (after the legal eagles have looked at HIPAA and laid down multiple forms a patient would have to sign prior to posting their own information on the web, especially if it’s a publicly available page).
Caregivers could then utilize the subjective portion while charting the objective portion online in the patient’s room during the visit.
Assessment and protocol could also be under the umbrella of caregiver management, as they currently are handled in the paper system.
Thanks to all for your kind words. Several weeks of noodling went into putting together this posting and I’m gratified to find that people are reading and finding it useful.
I’ll take a whack at some of your comments.
1) Randy and Steve raise questions about EXECUTION for GH — certainly a big challenge. You both wonder whether GH is Healtheon reincarnated.
What’s NOT different since Healtheon went public (around 1998)? Special interests are no less entrenched today, and I expect that there will be a lot of pushback. I’ve quoted Jim Clark before as pointing out that what many see as waste and excess spending in health care is what others see as food on the table. For every disrupter there is an disruptee.
Several things are different:
a) GH’s approach strikes me as far more collaborative and calculated. Healtheon was an Internet bubble company (IPO at $8, trading closes at $32 on day 1, height of the roller coaster at $120, then crashing down below original IPO price). The plan wasn’t there.
b) Healtheon’s model was primarily B2B, whereas GH seems to be banking much more on support from patients themselves, as well probably from employers, government, and others.
c) HIT developments in general, and the CCR standard in particular, have advanced significantly
These factors don’t guarantee success, but they raise the odds.
2) Simon and Paul raise the inevitable questions about TRUST.
My point here is not to defend GH, but I will share how I think about this. First, I’ll acknoweldge the validity of concerns about trust; this is a real issue.
For me it’s a risk/benefit analysis. The benefits of GH — both individually and for the health care system — are tremendous. The IOM pointed to 98,000 deaths per year in hospitals because of lack of quality and IT. Lack of IT in health care is a really big problem
On the risk side, I’ll pose back “Who would you trust” (In God we trust is not an option). While Google has baggage, so does everybody else on the trust issue — employers, health plans, pharma, others all have trust issues. Providers do better on trust, but they have little economic incentive to create interoperable, transportable PHRs.
3) Steve talks about Project HealthDesign’s evolving thinking about next generation PHRs. These guys have some great work around next generation PHRs — check out http://www.projecthealthdesign.org/ and http://rwjfblogs.typepad.com/pioneer/health_it/index.html . Steve correctly points out that an ecosystem is beginning to form around anticipated evolutions in PHRs.
4) Jen discussed SOAP and asks about the optimal EHR/PHR structure.
Think of the CCR standard as a foundation for PHI. In current form, the CCR standard covers free text, structured text, or coded data for 17 modules:
Patient demographics, Insurance information, Advance directives, Problems/diagnoses, Allergies and alerts, Medication list, Immunizations, Family history, Social history, Vital signs Results, Procedures, Encounters, Medical equipment, Plan of care, Health care providers, Functional status
As the MP3 of PHI, the current CCR standard is a great start…but there’s always MP4 for the future.
Vince
Great summary overview of Google Health’s possible business model by putting together the tidbits that Adam Bosworth has dropped at his various speaking engagements.
I was particularly interested in your outlook on the disruptive potential of Google’s PHI model on health plans. I just got done attending the AHIP Conference in Vegas and Google Health came up in alot of conversations with both the vendors/health plans.
If health plans truly do follow through on the buzzword of the conference (“B2C”), then Google’s PHI model poses a potential threat to health plans strategic initiatives to become “health care advocates” to their members on several fronts (primarily by negating the value of the large repositories of claims history data that the plans are sitting on).
With health plans already beginning to become under some pressure from banks on their one flank (financial transactions), I find it highly unlikely that they would agree to partner/share any data with Google and goes to great lengths to hinder Google’s efforts.
It would force Google to negotiate with a myriad of alternative partners (clearinghouses, PBMs, labs, etc) to supply them with personal health information. This would require a substantial strategic investment by Google in time, staff, and effort. I just don’t know if they will be committed to going down the rabbit hole into the health care industry.
Vince,
This is a terrific analysis. Thanks for pulling together these sources and commentary.
As to GH, all of us who have been around this industry and have seen numerous failures of “the next great thing” delivered by the non-healthcare IT world that promises to finally bring healthcare into this century. Nonetheless, we will root for the effort. While institional resistance to change will be a huge barrier to the GOOG, we may find that consumer apathy and fear (of loss of privacy) may be even more important. GOOGLE’s business success has been founded on fast consumer uptake and that source of energy will not drive this effort. GH will indeed have to demonstrate persistence until payors mandate electronically accessible records as a condition of participation and payment, and then the world will change.
GH – like every other EHR has to not only get the data but it has to be reliable, available, etc… Some of the most useful data is that which is not contained in the EHR but is locked up in outpatient devices. Getting this data into the EHR for use in clinical interventions will make a huge difference in outcomes.
We just presented our type 2 diabetes clinical trial results at ADA Scientific Sessions. I remember reading a comment about how there was no good data available yet in the world of wireless medical device enabled patient management. Well, here it is for type 2 diabetes.
I think the first thing most patients and providers will think about Google is who can “google” their PHR.
Google, Inc certainly has the industrial and IT clout to put something like this together, but the issue of PHR as a stand alone is inefficient….they need to develop a PHR that integrates into the system on separate servers which are secure (I am sure they thought about that one already)
I’ve referenced this article in a post on my site http://www.ehealthrisk.blogspot.com. Well done.
[…] Google Health will simultaneously create and dominate a new category of health offering: Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs […]
>>>>How will Google create sufficient critical mass to drive individual physicians to document clinical care in a PHR environment?
It bypasses physicians really, at least to start. Really it just relies on the billing data from the doctors, and we all know they like getting paid.
>>>>Simon put it very well…personally i find it bizarre to think patients will entrust Google.
It’s Google or Nothing ! Currently the patients don’t really have a seat at the Health Table.
>>>>Medical records aren’t the answer to everything
So true, exercise and clean drinking water saves more lives than any silly EMR.
Health plan sponsored PHRs are useless.
They have no content.
>>>>”Like all new things in today’s evolving consumer/retail healthcare industry, it will be the consumer and not the pundits like me who will eventually decide how successful Google’s strategy will be.”
If you believe this statement, you believe that Google will be very successful. Right now patients have little to no access to their health information. Google is going to MAKE THEM a part of the loop.
>>>>”Perhaps the ‘best’ or most useful PHR/EHR structure will not be a single EHR stored on a removeable memory stick (although wouldn’t that be handy???),”
PHRs on a memory stick will never work. I find it odd that someone could even think that they might.
>>>>”Simon and Paul raise the inevitable questions about TRUST. My point here is not to defend GH, but I will share how I think about this.”
Actually, over the long term, patients may feel there is *MORE* security having 1 place for all the health information vs. it being scattered ALL over the place ! Not to mention, a wee “theoretical security risk” seems small when the promise is of more organized, affordable healthcare.
>>>>”With health plans already beginning to become under some pressure from banks on their one flank (financial transactions), I find it highly unlikely that they would agree to partner/share any data with Google and goes to great lengths to hinder Google’s efforts.”
89% of the financial benefit of what I call exchangeable health information goes to the payors (health plans). read Markle.org
>>>>”I just don’t know if they (Google) will be committed to going down the rabbit hole into the health care industry.”
Good point. The healthcare pie *IS* big 🙂
Great post and comments on the potentials of Google Health. One other fact that might be useful is most EMRs are terrible and are unlikely to ever be able to exchange health information. So …. GH’s competition is weak, for the forseeable future !
Vince’s analysis, which is pretty close to my own, irons out a lot of the details. (link on THCB tomorrow, but great job)
The only way that I’d differ from Vince (other than I was too lazy to write my GH conclusions out fully) is that that I’d add in the one interesting VC investment Google has made. It’s in 23andme.
Aside from the fact that the CEO is Larry or Sergey (I can’t tell those two apart)’s wife—bet that made the pitch easier!— and that Esther Dyson has her hooks into it as well, the other interesting thing about 23andme is that it’s a genetic testing company. And it seems pretty logical that genetic information is going to be mixed into PHRs in the near future….so it doesn’t take a rocket genome scientist to make the link between 23andme and the not yet unveiled Google PHR/personal health URL.
They key question is whether Google (and more importantly American consumers using Google as a vehicle) has the clout to make the health care system willingly and easily give up its data….
We shall see.
One of the previous posting raised the scary prospect of big brother being able to google (I guess it is it a verb now)our Personal Health Records. Add in the prospect of someone being able to look at my genetic profile and we are talking about something real scary.
Let’s see..consumers already have a big trust issue when it comes to their personal health info. I wonder how they would feel if they thought their genetic profile could one day come up for sale in an AdSense text ad?
This is a great post and discussion forum on the topic of PHR.
I can not agree more that GH is one of the best positioned players to embark on the great IT and technological challenge to seamlessly syndicate and integrate scattered and non-standardized healthcare information for each individual.
One question, though, I have is, can “patient centric” be really feasible? The poor medical education level of general population tends to be blamed for the challenge, but more importantly, I am not convinced if the lifestyle modification and health management of an individual would require a whole depository of personal health information. Hence, I am not sure to what extent and exactly how GH would be able to leverage patients as a force to syndicate the scattered health data.
I would appreciate your insight.
[…] https://e-caremanagement.com/connecting-the-dotsgoogle-health-promises-to-create-and-dominate-next-ge… […]
[…] you are interested in Google PHR you should read Vince Kuraitis post titled “Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs̶… and the discussion it has been generated. Congratulations for such a wonderful post and for the […]
But will anyone trust them with their PHI?
Google make money by taking other people’s data and selling it to advertizers. Do you trust them with your PHI and do you want them selling your deidentified data to the health care providers and drug companies (and government?) to make money.
There is also a community model where people engage in a discussion about health topics. PHI sharing comes as trust is established – which can be monetized also through advertizing – the sort of MySpace for health care. Perhaps the bootstrap will involve “Dr. Google” or his agents providing expert, trusted advice. The agents should be associated with trusted real-world health care brands until the conversation floats into the virtual world and on-line reputations take over.
If tusted health care brands got a clue and they’d enter the market themselves and compete with Google. They (badly) understand HIPAA and protect patient data like it was their own. And their buiness models are at least based on delivering something or real value – care. But it probably won’t happen since they neither have the technology skills nor the vision.
If Google are only partially successful it will still be a boon to consumerism by getting outcome information into the hands of the consumer to support personal choice. It will also put pressure on the medical profession who seem to want to make “doctoring” a secret secience of the well-qualified, with the patient positioned as too ignorant to know what’s best for themselves.
Great study but presumably Microsoft is also a player here.
They recently acquired Azyxxi(an aggregator of hospital-wide EMR data) and Medstory(a content provider now linked with MSN).
Wildcat will follow shortly https://www.microsofthealthbeta.com/shell/help.aspx?topicid=faq
I think they will take a more pragmatic approach to solving the need for standardization and pulling together scattered data for a PHR given their entry into the EMR alrady.
In terms of the business model – I think the % of the population that will actually use a PHR is limited. Most people don’t want to be reminded of their mortality and a record of your health is a nasty reminder. Checking the value of your stocks and social networking is a far nicer way to spend time online for most people.
[…] blogChronic Disease Management • Technology • Strategy • Issues and Trends « Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs | Main “In God We Trust” is NOT an Option for Your PHR: 5 Responses to the Google […]
if there is a PHR system only, it will be no value for consumer.I think the PHR system not only includes the alert or reminder,but also health promotion programs.
In China,the Google will have no choice.I feel sorriness.
Oh well
Electronic health reords aren’t the magic bullet after all.
Stanford shows no improvement in patient care due to electronic health records:
http://news.yahoo.com/s/nm/records_dc;_ylt=AlxlcRLgG13iGzBvV1SoWIPq188F
Excellent logic and conclusive arguments, Vince. I’ve been tracking PHRs and watching Google (and Microsoft) for a long time now, wondering where they’ll strike. No, they’re not the only ones pursuing this challenge, but both of these companies have the critical element holding back other groups (especially those working through SDO SIGs)–and that, of course, is funding. The Google and Microsoft approaches may not be perfect, but at the moment, they have more to offer than anyone else out there.
As part of my tracking, I’ve tried out various PHR models. And, as someone has already said, the USB-based flash drive key is not a good-enough solution. However, what do you think about CapMed’s recent acquisition and plans to put PHR data on cell phones? This might put enough information at hand for those who need vitals, for example, but I can’t imagine much depth. (But I don’t have an iPhone, either)
As part of his excellent piece, Vince K. reminds us of the exacting requirements of full-service PHR success. Perusing these requirements (it’s a Friday afternoon in Boston in the middle of summer, but here I am, perusing in full gear. Vince, you owe me) suggests to this grizzled observer a disquieting conclusion: Google is not big enough for this job. Hoping that Google can bring sanity single-handedly to health care is like hoping the US can bring peace single-handedly to Iraq. You’re big, baby, but you ain’t that big.
So Vince, my main man, you need to bump your analysis up a level. Who or what is bigger even than Google? The self-same US of A, that’s who! Take your terrific essay, Find every mention of “Google” and “GH,” hit Replace and substitute the words “federal government,” and you got yourself a plan!
Yessirree bob, I propose that e-CareManagement convene a serious discussion of the only truly scalable solution to the woes of US health care — national government mandates. If they’re good enough for Social Security and good enough for Medicare, they’re dang-tootin’ good enough for PHRs! A lot of Democrats know I’m right but aren’t ready to say so yet, know what I mean? But it’ll come! The Kuraitis plan for national PHRs, right-sized, federalized, and deGoogle-ized!
Very thought provoking blog about exciting innovative times ahead. My main concern with the blog is that the contains an inaccurate statement about lack of HIT standards. If you had said that the standards are not yet widely adopted, that would be accurate. It is also a fact that “ALL” the standadrs for HIT have not yet been identified. But the specs for “Consumer Empowerment” including exchange of the data included in CCR (using the APPROVED, not future, HL7 CCD XML specification) have existed for nearly a year, were created through an open multi-stakeholder public process (not unilaterally) and were accepted by ANSI HITSP and HHS. HITSP’s interoperability specs include the coding standards that the blog (incorrectly) says are missing. Those accepted standards are in existence and in process of being implemented. Thus, rallying around those standards would help both providers who have EHRs, as well as patients who have PHRs (Google’s or other) to all be interoperable without divergent and wasteful efforts.
Creating “de facto” standards might get the ball rolling if “de jure” standards didn’t already exist, but now the best course is for “de facto” and “de jure” to be one and the same.
[…] though still a mystery, caught the attention of Vince Kuraitis back in June — causing him to write about what he thinks it may look like based on hints dropped in those presentations. His article is a […]
[…] Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs – e-CareMan…: “Google Health (GH) could be the event of the decade in advancing health care reform — not just healthcare information technology (HIT) reform, but health care system reform. GH promises simultaneously to create AND dominate the market for next generation personal health records (PHRs). There is nothing else in our solar system or in the entire universe like it.” […]
[…] wants to be ‘the’ company of the millennium and beyond, especially with it [Google] courting medicine. Without a doubt that you will within 10 years see Google as the dominant force in ALL advertising, […]
This is terrific initial analysis and discussion! I’m glad to see that being patient-centric is one of the key elements, though the devil will be in the details of how this is carried out. I have two points that I don’t think have been raised yet and on which I’d like further comments from others.
One, there are a couple of bills floating around Congress to support the establishment of Independent Health Record Banks (also sometimes called Independent Health Record Trusts). A key facet of these banks is that the persons whose data are in the bank are the only members of the bank and have ultimate say over policy for the bank. While this puts the “patients” individually and collectively in a position of control that appears to me to be stronger than others models that I’ve seen, I’d be interested in comments on how such a bank seen as a variant of a PHR’s database, would work in practice to accomplish this sort of patient-centric result without seriously denting the interests in a business model to fund the operations. Would this level of control encourage more patients to use/support useful health data sharing?
Two, most privacy laws/regulations today govern the sharing of data between health enterprises and support the right of patients to obtain their health information and use it as they wish. By one theory, if the data that might usefully flow between health enterprises used the patient (or patient-controlled agent) as an intermediary, then the patient would have control over his/her health information flow in a way that would seem to eliminate the typically complex decision about whether sharing the data was permitted under law. Generally, it seems that the question for a health enterprise would turn from “Can I release this data without risking violation of a privacy law/regulation?” to “Is there a solid rationale for me to resist releasing this data?”. While such a model would move some power from health care enterprises to their customers (and so they may resist), it seems to be consistent with the idea of a patient-centric model generally and seems to solve the sharing problem to most customer’s satisfaction. How do you see the future of this idea?
Wow. And nowhere do we ask about the millions of people with no internet access, or who are not technology-compatible. How does this “reform” the fact that we consider healthcare something that people must “earn” to receive. That a doctor’s attention is something one has to deserve? That economic losers should just curl up and die?
How, in fact, does this change anything, aside from improving the records of a majority-elite and sorta-kinda-not-really control costs? Not that there’s anything wrong with that, but I can’t help but feel this will be just another reason to discriminate against the poor – no EHR? Sorry. I don’t see patients without them.
[…] Google and PHR […]
[…] pieces that add up to this possible future come from e-CareManagement and The Health Care Blog. At e-CareManagement, Vince Kuraitis wrote at length about the various […]
Please keep me informed about this.
Vince, Adam Bosworth has left Google. Any insight on the future of Google Health?
[…] Connecting the Dots?Google Health Promises to Create AND Dominate Next Generation PHRs – e-CareManag… – What is Google up to? […]
Asako, your question about “now what, given that Adam Bosworth is leaving” is right on target.
Adam seems to have been the driving force behind Google Health to date. Anything I said about the future would be totally speculative, so I’ll just say that I hope his vision has been ingrained with the remaining members of the team.
Vince
[…] what drugs I am on? And, even if I do, do I care? I don’t think I do as long as the PHR (or whatever tool) is always available to me and my care […]
I think Google may be finally stepping over the invisible line of privacy norms. We already essentially gave Google our personal email (Gmail) and information on all our friends (Orkut and Facebook) and what we want (Search History, Froogle, Shopping)… now they are talking about the last barriers to privacy really. But who knows, it might be that technology has officially killed privacy.
At CureHunter we are patient activist oriented too, but rather than asking for their data we stick with analyzing peer-reviewed research. Disease research is complicated enough without adding more human data-entry error into the mix.
I think we need a national/global initiative to standardize the exchange of anonymous data between hospitals… first. The hospitals still have the best data.
[…] he did with Google’s PHR, talking even about trust issues, Vince Kuraitis analyzes Microsoft’s HealthVault and four […]
Maybe contract law could help patients enhance the privacy of their health records. http://hack-igations.blogspot.com/2008/02/contracts-for-patient-privacy.html
It occurs to me that this situation (clearinghouses for PHI) is not entirely different from that of credit reporting bureaus. Financial information is a close second to health information, in my opinion, in the importance of privacy.
However, there are for-profit firms who aggregate, and dispense this information in an expedient way. This has allowed a great deal of efficiency and speed in the retail banking world. Consumers must consent to the collection, and ultimate dissemination of their financial info before it can be shared.
I don’t see how google health is much different. nothing happens that the patient does not ultimately allow.
Frankly, I’m all for it because in the end, it is the choice of the consumer, and the consumer has complete control.
I agree that there needs to be much better organization in health care records. I work in the field and I am blown away by how little people actually keep track of as it realtes to their own care. If you ask when did you ahve that surgery most take a guess & do not keep any record this coupled with teh fact that the health care system is soooo far away from being able to share information is why I now keep all of my & my families health care information in software called MyMedTracks by a company called HomeTreeTech. For 24.95 plus shipping you can get a copy of this amazing software & put all of your familes records in one place. Now when I go to the doctor I have a reference of all of my surgeries, medications and other importnant info. at my fingertips. This has been a lifesaver. I do commend goggle and others working on this problem – when I asked my Dr. about this he said that he is not ready to share his information online & I agree. Thanks for the great explanation on this!!!!
Wow, where to start…First of all you did an excellent job with this essay and you make a strong argument for google health but I still don’t like the idea of google having that much information. I think it’s one of those things that can easily end up out of control. I’m all for health care reform for sure, as we are the richest nation in the world and yet people still die to this day from lack of common medical treatment, so I’m all for it. But google is going to give me the creeps pretty soon. Kind of ‘big brother’ like.
DELI Connecting the Dots…Google Health Promises to Create AND Dominate … http://tinyurl.com/2tfdwv
RT @tweetmeme Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs | e-CareManagement http://bit.ly/2sap8d
http://tinyurl.com/6hytp4
Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs
Connecting the Dots…Google Health Promises to Create AND Dominate Next Generation PHRs http://t.co/i8Vse9v