Subscribe if you want to be notified of new blog posts. You will receive an email confirming your subscription.

Which Platform of Platforms (UDHP) is Right for your Health System? A Market Analysis
By Neil P. Jennings and Vince Kuraitis
In previous posts in this series, we have covered the definitions of Unified Digital Health platforms and whether “EHRs can become UDHPs.” In this follow-on post, we’ll talk through the requirements for success for a UDHP and which types of healthcare organizations are best suited for which types of UDHPs. This post will build on findings from the previous posts.
The Market Needs UDHPs: Key Takeaways from Previous Posts
Key Takeaway 1: The healthcare industry needs UDHPs to create a centralized, common architecture for healthcare organizations
Key Takeaway 2: The healthcare organizations leveraging UDHPs will achieve a myriad of benefits, from competitive advantages to clinical, financial, and operational gains
Key Takeaway 3: UDHPs are not all-or-nothing or mutually exclusive from EHRs. As we explored in our last post, EHRs could expand into UDHPs. These EHRs as UDHPs (or the relative platform of platforms) may be the optimal choice for some market segments. EHRs may also be accommodated into cloud-first UHDPs.
Key Takeaway 4 / Guiding Criterion: This post will focus on US regional and local health systems and outpatient groups of all sizes.
The Approach: Market -> Segments -> Options -> Fit
- For this post, we will start from the top-down market perspective, analyzing the overall market landscape.
- Once we have described the landscape, we will call out the key segments (organization types, sizes, and profiles) that we will be evaluating.
- At this point, we will approximate IT budgets and IT team sizes by organization type to determine capabilities of building as opposed to depending on partners and vendors.
- Then, we’ll review the constraints for implementation and ownership, outlining the drivers of UDHP fit.
- Next, we’ll break down the different ways UDHPs can be developed and maintained.
- Leveraging an EHR as UDHP
- License from UDHP vendor
- “Home grown” cloud-first solution
- Finally, we’ll crosswalk the segments and the optimal option for each segment, based on their specific needs and estimated IT and budgetary resources.

Can EHRs Expand to Become Health Systems’ “Platform of Platforms” (UDHPs)?
In a previous post in this series, we discussed healthcare’s migration toward Unified Digital Health Platforms (UDHPs) — a “platform of platforms.” Think of a UDHP as healthcare’s version of a Swiss Army knife: flexible, multi-functional, and (ideally) much better integrated than the drawer full of barely-used apps most health systems currently rely on.
We included a list of 20+ companies jockeying for UDHP dominance, including two familiar EHR (electronic health record) giants — Epic and Oracle. This raises the obvious question for today’s post:
Can EHRs level up into becoming UDHPs — becoming healthcare’s platform of platforms? Or are they trying to wear a superhero cape while tripping over their own cables?
We see good arguments pro and con, and like most things in healthcare “it’s complicated.” Some say EHRs are uniquely positioned to make the leap. Others believe the idea is like trying to teach your fax machine to run population health analytics.
Thus, we’ll lay out the arguments for differing points of view, and you can decide for yourself. Here’s an outline of today’s blog post:
- A Brief Recap: What are UDHPs?
- Thesis: EHRs Can Expand to Become UDHPs
- EHRs Currently Own the Customer Relationship
- Many Customers Have an “EHR-First” Preference for New Applications
- Epic and Oracle Health are Making Strong Movements Toward Becoming UDHPs
- Antithesis: EHRs Can NOT Become Effective EHRs
- EHRs Carry a Lot of Baggage
- Customers are Skeptical
- EHR Analytics Are NOT Optimized To Achieve Critical Health System Objectives
- EHR Switching Costs are Diminishing
- Cloud Native Platforms Accelerate Innovation and Performance
- It’s Not in EHR DNA to Become A Broad-Based Platform
- Synthesis and Conclusion

Webinar — Platform Shift: What is Beyond EHRs?
Our recent blog post “Platform Shift: From EHRs to UDHPs (Unified Digital Health Platforms)” has attracted a lot of attention. We’ll share highlights of the post and answer your questions in an upcoming webinar on Monday, April 28, at 1:00 PM Eastern time.
Jose Garcia will moderate a discussion among Girish Muralidharan, Jody Ranck, and me (Vince Kuraitis).
Register for the event by clicking on this link. Remember to use LinkedIn’s “Add to calendar” feature when you register. A recording will be available after the event.
Some of the 𝐭𝐨𝐩𝐢𝐜𝐬 𝐰𝐞’𝐥𝐥 𝐝𝐢𝐬𝐜𝐮𝐬𝐬:
- Why does healthcare need a “platform of platforms”?
- What are UDHPs (Unified Digital Health Platforms)?
- What are value propositions of UDHPs?
- What are examples of UDHPs? We’ll discuss two – 1) ServiceNow, a vendor case study, and 2) Mayo Clinic Platform, a healthcare provider case study
- What are some business and strategic implications of UDHPs? We’ll reference six.
Hope to see you there!
Platform Shift: From EHRs to UDHPs (Unified Digital Health Platforms)
by Vince Kuraitis, Girish Muralidharan*, and Jody Ranck*
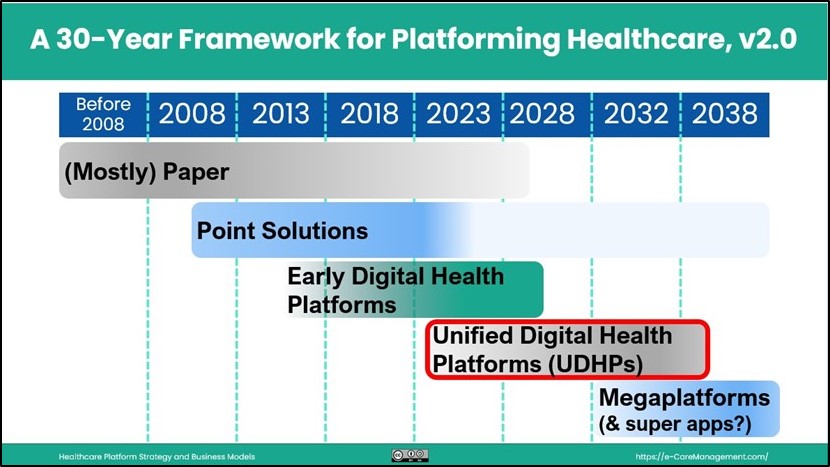
This essay is the next in the series entitled “Platforming Healthcare — the Long View”. The series presents a 30-Year Framework for Platforming Healthcare. An updated v2.0 of a graphic depicting this 30-Year Framework is shown above.
Today’s post will describe and discuss a potential successor to the EHR era — Unified Digital Health Platforms (UDHPs). Here’s an overview:
- Background and Environmental Trends
- Gartner’s Key Role in Characterizing the UDHP Movement
- UDHP Value Propositions
- Examples of UDHPs
- ServiceNow
- Mayo Clinic Platform
- Business and Strategic Implications of UDHPs
- APPENDIX: Additional Readings on UDHPs
This is a long post – about 4,000 words. So grab a cup of coffee and dig in.
*Disclosure: Girish Muralidharan previously worked at GE Healthcare, a UDHP vendor. Mayo Clinic Platform was a client of Ranck Consulting.
Background and Environmental Trends
Healthcare is fragmented. Data is not standardized and has existed in silos. Patients and clinicians have disjointed experiences. Payment structures create conflicting incentives.
Electronic Health Records (EHRs) were once touted as the key solution for transforming healthcare to a modern, digitally-enabled industry. Yet, they continue to frustrate clinicians with poor UI/UX and largely fulfill a primary role as a system of record to document claims submissions.
Recent technological and business trends have begun transforming healthcare into a more unified and integrated experience:
- HITECH (in the U.S.) drove the adoption of electronic health records across the industry
- Standards-compliant data models and APIs across various solutions are allowing third-party integrations to add new functionality
- Value-based care (VBC) and value-based payment (VBP) models incentivize improving quality rather than maximizing fee-for-service volumes
- AI’s emergence and adoption in healthcare fuels the need for more – and better – data and data liquidity.
- New competitors in healthcare (Big Tech, Big Retail, digital health ventures) compete based on improving patient experience, advancing VBC and VBP models, and integrated data and analytics
- Accessible cloud computing infrastructure is enabling a plethora of **-as-a-Service business models
Healthcare organizations want integrated solutions, not more point solutions. See the previous blog post in this series — “Beyond Awareness: Understanding the Magnitude of Point Solution Fatigue in Healthcare”.

Gartner’s Key Role in Characterizing the UDHP Movement
The trends and forces listed above open the door and create the need for a new category of enterprise software – Unified Digital Health Platforms (UDHPs).
A December 2022 Gartner Market Guide report characterized the long-term potential:
The DHP shift will emerge as the most cost-effective and technically efficient way to scale new digital capabilities within and across health ecosystems and will, over time, replace the dominant era of the monolithic electronic health record (EHR).

The ConV2X Conference: Blending Platforms for Patient and Enterprise Success
I want to make sure you’re aware of an in-person event at which I am speaking – the 8th annual ConV2X Blending Platforms for Patient and Enterprise Success in Healthcare & Life Sciences, September 10 and 11, Quincy, MA, USA.
About the ConV2X Conference
ConV2X is short for ConVerge-2-Xcelerate – an annual event that informs audiences with high-value education, discussion, and information about trends on the horizon.
The 2024 theme is “Blending Platforms for Patient and Enterprise Success.” This is the leading C-Suite conference focused on platforms, AI, and decentralized technology — bringing together global industry authorities to this 2-Day event.
More info about speakers, topics, and the agenda: click here.
Dates and Times:
September 10, from 10 AM – 9 PM ET
September 11, from 8:00 AM – 3 PM ET
Place: Kilroy Square | 1492 Hancock Street | Quincy, MA, 02169 USA
Register here and get a 15% discount!
About My Presentation (September 10)
Title: Your company has a technology platform…but do you have a platform business model and strategy?

Beyond Awareness: Understanding the Magnitude of Point Solution Fatigue in Healthcare
Healthcare is saturated with point solutions. A February 2024 report by Galen Growth and Finn Partners documented that there are over 14,000 digital health ventures worldwide. Tracxn reports that there are nearly 3,500 healthcare AI startups in the U.S. alone.
The problem of point solution fatigue is widely acknowledged in healthcare. The unique contribution of this post will be to document the magnitude of the challenge and to explain how we got here.
This post is #2 in a series on “Platforming Healthcare — the Long View”. The first post presented A 30-Year Framework for Platforming Healthcare. Here’s the roadmap to today’s post:
- The magnitude of point solution fatigue in healthcare
- The patient POV
- The health system POV
- The employer and health plan POV
- Are point solutions appropriate in some circumstances? Yes!
- How did we get to point solution fatigue?
- Conclusion
- APPENDIX: A visualization of healthcare’s point solution fatigue
The Magnitude of Point Solution Fatigue in Healthcare
Point solutions are uniquely problematic in healthcare:

A 30-Year Framework for Platforming Healthcare
Healthcare has a reputation as being one of the most complex and fragmented industries. I’ll bet you’ve spent time pondering how we get ourselves out of this mess. This post is first in a series that takes a long-view perspective on platform adoption and evolution in healthcare. I’ll start by sharing Version 1.0 of “A 30-Year Framework for Platforming Healthcare” — see the graphic above.
A few weeks ago I was interviewed by Ruta Gabalina and Aiym Sarmanova of PPMI, a leading European research and policy analysis center. They are working on a study exploring the evolution of platforms in healthcare.
I shared my framework with them verbally, and now I say “thanks” for their creating a v1.0 graphic. It’s rough…gotta start somewhere 😐. I’ll greatly appreciate your reactions and suggestions for v2 and beyond.
Let’s take a look at the time frames listed in the graphic. The phases are not discrete — think of them as overlapping
Before 2008: (Mostly) Paper

“The Point Solution Paradox” in Healthcare’s Adoption of AI
AI adoption in healthcare is facing “The Point Solution Paradox”. This paradox highlights the intricate balance between the necessity of point solutions in the evolution of AI in healthcare and the challenges they pose in an already fragmented industry.
Here’s a roadmap to this post:
- Investment and innovation has been dynamic, but adoption lags
- A 3-phase framework for AI adoption
- The Point Solution Paradox
- Care providers prefer integrated solutions
- A case study of The Point Solution Paradox: medical imaging
- How will The Point Solution Paradox play out in healthcare?
This blog post is the first in an occasional series examining the synergies between AI and platforms.
Investment and Innovation has Been Dynamic, But Adoption Lags
The digital health landscape has been dynamic. A 2023 report by FINN Partners and Galen Growth documented that there are over 9,000 digital health ventures worldwide. An analysis by Tracxn estimated that there are over 3,147 AI startups in healthcare in the United States alone.
However, the adoption of AI in healthcare has lagged for varied reasons. For example, an August 2023 report by Bain and Company found that only 6% of health systems have a generative AI strategy.
Thus, a pivotal question arises: How will future AI adoption unfold in healthcare?

The Mathematical Imperative for Platforms in Healthcare
Network mathematics explains the imperative for platforms in healthcare.
There are only two ways to make connections in a network — i.e., ways to connect the diverse nodes in a network. The first is through point-to-point connections. A simple diagram (below) provides an example of the math. Here there are six different participants in a healthcare network. If you rely on point-to-point interfaces – such as email, fax, phone, in-person contacts – there are 15 possible connection points to make.

In a point-to-point network, as the number of nodes in a network increases linearly, the number of possible connection points increases exponentially.
The connections between the nodes can represent potential communications, actions, or data transfers. You can also think of the connections as potential failure points in a network — where communications, actions, or data transfers should happen but don’t.
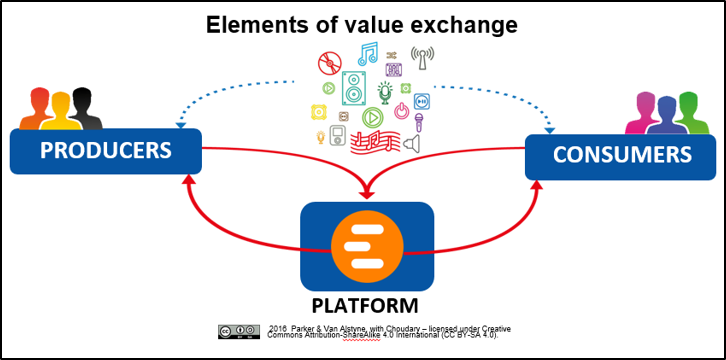
The other way to connect nodes – or people – in a network is through a network hub — a platform.
Your Company Has A Technology Platform…But Do You Have A Platform Business Model and Strategy?
Today in healthcare, platforms are understood mostly as technology. That’s not wrong, but it’s limiting and it misses a huge opportunity to adopt a platform business model.
In most other industries platforms are also understood as a business model and strategy. Outside of healthcare, there are 45+ books focusing on this topic.
This post is written for:
- 9,000+ early-stage digital health companies, most of which have a software and/or hardware technology platform as a centerpiece of their offering
- Healthcare incumbents — health systems, health plans, pharma, medical devices, etc. — that provide a digital platform as part of their external offering. For example, health systems that have an EHR platform, a patient portal, and/or a population health platform.