Subscribe if you want to be notified of new blog posts. You will receive an email confirming your subscription.
Beyond Awareness: Understanding the Magnitude of Point Solution Fatigue in Healthcare

- A 30-Year Framework for Platforming Healthcare
- Beyond Awareness: Understanding the Magnitude of Point Solution Fatigue in Healthcare
- Platform Shift: From EHRs to UDHPs (Unified Digital Health Platforms)
- Can EHRs Expand to Become Health Systems’ “Platform of Platforms” (UDHPs)?
- Which Platform of Platforms (UDHP) is Right for your Health System? A Market Analysis
Healthcare is saturated with point solutions. A February 2024 report by Galen Growth and Finn Partners documented that there are over 14,000 digital health ventures worldwide. Tracxn reports that there are nearly 3,500 healthcare AI startups in the U.S. alone.
The problem of point solution fatigue is widely acknowledged in healthcare. The unique contribution of this post will be to document the magnitude of the challenge and to explain how we got here.
This post is #2 in a series on “Platforming Healthcare — the Long View”. The first post presented A 30-Year Framework for Platforming Healthcare. Here’s the roadmap to today’s post:
- The magnitude of point solution fatigue in healthcare
- The patient POV
- The health system POV
- The employer and health Plan POV
- Are point solutions appropriate in some circumstances? Yes!
- How did we get to point solution fatigue?
- Conclusion
- APPENDIX: A visualization of healthcare’s point solution fatigue
The Magnitude of Point Solution Fatigue in Healthcare
Point solutions are uniquely problematic in healthcare:
- Complexity and Integration Challenges: The integration of multiple point solutions can be highly complex, leading to workflow and interoperability challenges. IT departments have to evaluate, implement, manage, and monitor multiple solutions.
- Regulatory and Compliance Risks: Navigating the regulatory landscape and ensuring compliance adds another layer of complexity for healthcare organizations.
- Fragmentation of Care: The lack of integration among point solutions can result in a fragmented patient experience, where individuals struggle to manage their health across multiple, disconnected platforms and applications.
- User Adoption and Training: Healthcare providers face challenges learning and adapting to various user interfaces and workflows, leading to frustration and resistance to adoption.
- Cost and ROI Concerns: The financial burden of implementing and maintaining multiple point solutions is significant, often making it difficult to demonstrate a clear return on investment (ROI).
Let’s take a deeper look at how point solutions affect patients, health systems, employers, and health plans.
The Patient POV

As documented in a Change Healthcare and Harris poll, patients are bewildered by their overall experiences with the U.S. healthcare non-system. Additional findings from the poll:
- 62% believe that “the healthcare system feels like it is set up to be confusing”
- 81% believe that “shopping for healthcare should be as easy as shopping for other common services”
Consider the challenge from a patient’s point of view. Suppose you’re a 60-year-old black, gay man with diabetes and asthma. Which digital health point solution should you choose for your care?
- The one targeting men?
- The one targeting seniors?
- The one targeting black patients?
- The one targeting the LGBTQ community?
- The one focusing on diabetic patients?
- The one focusing on asthmatic patients?
- More than one? which ones?
Smartphone apps further compound patient confusion. IQVIA has reported more than 350,000 mHealth apps.
I’ve written an entire series of posts on the failures of today’s patient portals. A few highlights:
- By definition, today’s portals are NOT patient-centric — they are tethered to individual provider organizations.
- 86% of patient survey respondents answered that the single greatest use of a portal was simply to review test results — vs. coordinating and improving long-term patient care.
- A survey of hospital execs found that 94% believed the single greatest benefit of the patient portal was “accepting patient payments”. Only 35% saw value in involving patients in their clinical care.
- Today’s patient portals can only capture stand-alone value, NOT network value.
- Today’s patient portals have high friction across multiple portals.
- Today’s patient portals miss out on network effects.

A survey conducted by PYMNTS and Lynx confirmed the obvious: “Approximately four in five consumers are interested in using a unified digital platform to manage information about their care and insurance benefits.”
The Health System POV
55% of hospital execs receive more than 11 vendor calls and emails from digital health solution vendors per week. —pandahealth, Hospital Digital Health Technology Report 2022
In 2023, symplr surveyed health system clinicians and CIOs. They found that a majority (55%) of respondents still use between 50 and 500+ software solutions to run their organization’s healthcare operations.
Does 500 software solutions strike you as a lot? Here’s one example of a health system with many more than that:
We started off with about 1,600 give or take. These are main departmental apps, enterprise applications…In about the past 24, 30 months or so, we’ve gotten rid of about 500 applications. I’m trying to get rid of another 500 over the next 24 to 36 months and consolidate our application tech stack to maybe around five or six hundred total apps for the health system. —Aaron Miri, Chief Digital & Information Officer, Baptist Health System
Can it get worse?
There are health systems we walk into that have over 3,000 different point solutions and technologies that they’re supporting. —Kristen Valdes, CEO b.well Connected Health

As detailed in the 2022 symplr Compass Survey Report, more than 88% agreed that working with disparate technologies complicates their job.
The Employer and Health Plan POV

There is a technology solution for every possible issue you might consider. And so it can be a little bit overwhelming. I don’t know if your inbox looks like mine, but three quarters are from, external vendors that have great things they want to pitch.” —Krista Hoglund, CEO Security Health Plan
I’ve combined employers and health plans together because they have similar (albeit not identical) challenges in providing health solutions for 3rd party employees or plan members.

Here’s how Christina Farr and Peter Hames spell out the employer’s POV:
A decade ago, any sensible founder of a digital health company in the U.S. would have considered targeting the self-funded employer market. It would have been an oversight not to. It’s easy to understand why. Faster moving than health plans, with sizable populations and healthcare spend that can run into the billions, they were attractive buyers. Employers were hungry for solutions that could potentially bend the cost curve in health care, given rising rates of medical inflation. But, unlike health plans, they were motivated by more than just minimizing their “loss ratio” of paid-out claims – they wanted to attract the best employees with eye-catching, competitive benefits, and proactively keep those employees happy, healthy and productive.
Their recommendation is to “avoid going all in on self-insured employers — with a few notable exceptions…here’s why:
- The competition and noise are intense
- Vendors are now expected to share risk
- Most solutions don’t address a need that is broad or expansive enough
- The market is populated by mature incumbents
- There’s a war for good commercial talent
- Benefits consultants/brokers are under greater scrutiny”
MedCity News reported:
It is not uncommon for health plans and employers “to have upwards of 20 point solutions. That means juggling a dozen or more different vendors, all of which will likely have their own branding as well as company-specific technology and workflows for marketing and communicating with members. None of these point solutions talk to each other. It’s like having to buy a different cell phone for each contact.”
A survey from Quantum Health found that HR leaders spend 1/3 of their average workweek managing benefit point solution vendors. Among large employers, 69% are worried about siloed care experience for employees and 60% are concerned about lack of integration between vendors.
Are Point Solutions Appropriate in Some Circumstances? Yes.
Point solutions are a prime source of innovation in healthcare — they address specific challenges with targeted solutions.
To be sure, there are circumstances in which point solutions are appropriate:
- Addressing specific needs or gaps
- Rapid deployment and results
- Limited budget and resources
- Testing and experimentation
- Regulatory compliance
- Scalability in stages
- Integrating with legacy systems
Point solutions are also a NECESSARY first step in the broader adoption of general-purpose technologies, such as artificial intelligence. For an in-depth explanation, see my recent blog post: “The Point Solution Paradox in Healthcare’s Adoption of AI.”
How Did We Get to Point Solution Fatigue?
What’s happened in the past 15 years to fuel the surge of point solutions?
HITECH EHR funding. In 2009 the U.S. was still reeling from The Great Recession Healthcare had barely begun becoming digitized;.less than 10% of hospitals and less than 20% of physicians had an EHR. Congress appropriated $35 billion for EHR adoption, and by the middle of the 2010s 95% of hospitals and nearly 80% of physicians had adopted an EHR.
An influx of capital and low interest rates. VCs and PE firms “discovered” digital health in the early 2010s and poured $100 B+ into early-stage companies.
Big Tech and Big Retail invade healthcare. Before 2009, Big Tech and Big Retail had not yet entered healthcare in a significant way. Over the next decade, nearly every major tech and retail company entered the healthcare space.
Unique healthcare pain points and/or areas of innovation. Here are a few examples of point solution offerings that were developed to meet areas of high need or pain:
- Improving patient experience
- A focus on revenue cycle management
- COVID fueling the adoption of telehealth, virtual care, and home care offerings
- AI — both predictive and generative AI
The APPENDIX below presents a partial visual display of the explosion of new offerings in healthcare.
Conclusion & Summary
The magnitude of point solution fatigue in healthcare is undeniable. As the industry grapples with thousands of specialized tools, the resulting complexity, fragmentation, and inefficiencies highlight an urgent need for more integrated solutions.
Future posts in this series will examine topics such as
- A closer look at the emerging category of Unified Digital Health Platforms (UDHPs) — what are value propositions, who are players, etc.
- Are EHRs a potential solution to point solution fatigue? Could EHRs function as Unified Digital Health Platforms (UDHPs)?
- What if you’re a healthcare point solution company? What are strategies/tactics to consider in a new environment where customers prefer integrated offerings?
- Version 2 of “A 30-Year Framework for Platforming Healthcare”
If you have a few more moments, please continue scrolling through the graphics in the Appendix below.
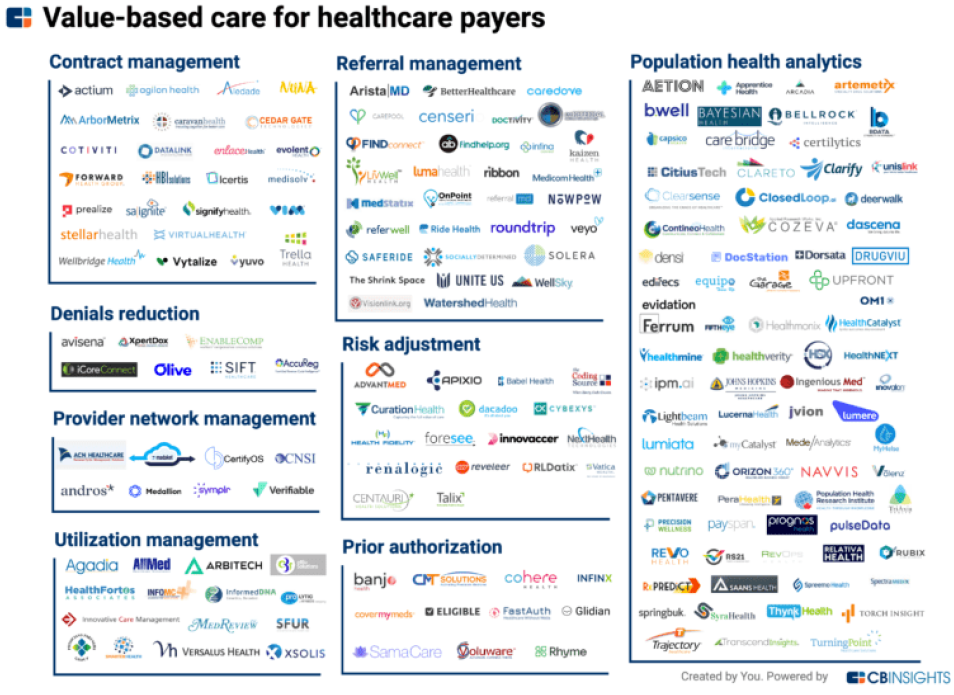
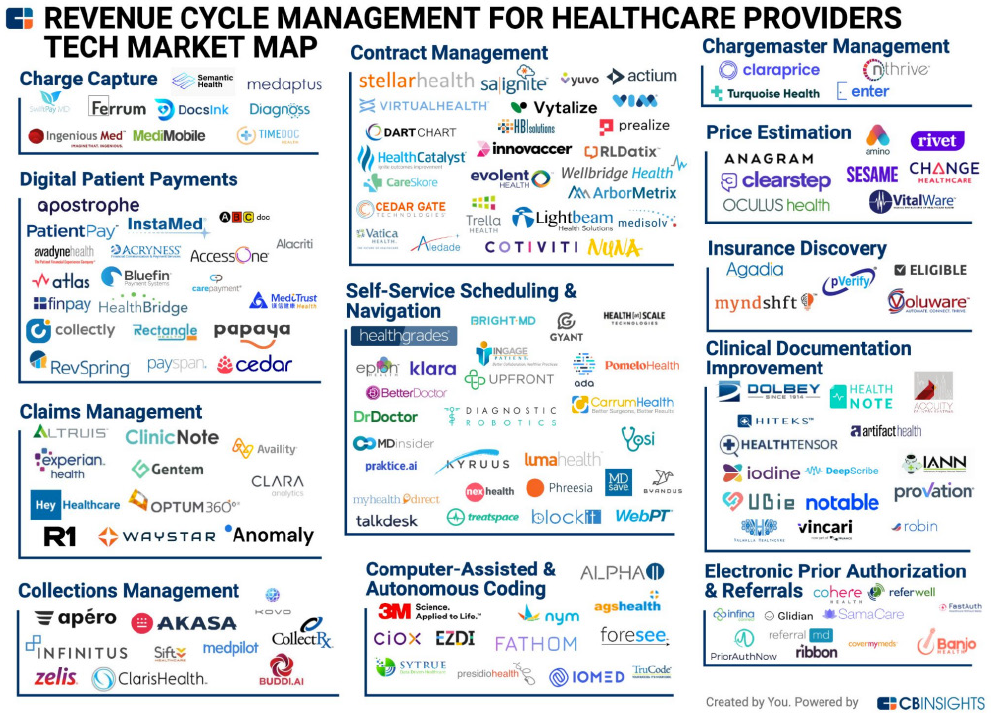
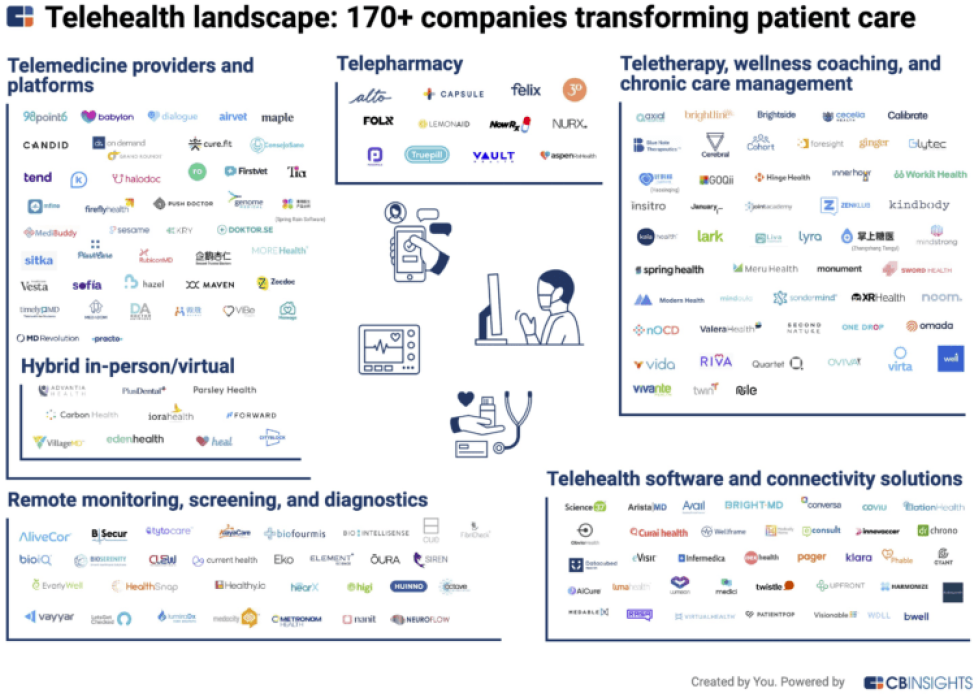
APPENDIX: A Visualization of Healthcare Point Solution Fatigue
Sometimes a picture is worth a thousand words.
The CBInsights Book of Market Maps presents a number of categorized “maps” of early-stage companies in healthcare. The CBInsights book is available as a free download.
Scroll down to view a fraction of today’s 14,000+ global digital health ventures.
























This work is licensed under a Creative Commons Attribution-Share Alike 3.0 Unported License. Feel free to republish this post with attribution.