Subscribe if you want to be notified of new blog posts. You will receive an email confirming your subscription.
EHR 2.0: Thinking Outside the Cat Box
 One of the potential dangers of limiting $17 B HITECH federal stimulus funds to electronic health records (EHRs) is the risk of locking-in outdated technologies. Let’s consider what this might mean.
One of the potential dangers of limiting $17 B HITECH federal stimulus funds to electronic health records (EHRs) is the risk of locking-in outdated technologies. Let’s consider what this might mean.
If you think of today’s EHR technology as EHR 1.0, what might EHR 2.0 look like? This post presents a number of innovative ways to conceptualize EHR 2.0:
- EHR as Platform + Applications
- EHR as Clinical Groupware
- EHR Integrated with PHR
- EHR as Software-as-a-Service (SaaS)
- EHR as a “Publish-Discover” Search Engine
- EHR + Disease Management Services = Care Coordination
- DRT-Enabled EHR
My point here is not to provide an exhausting listing of what’s possible, but simply to get you to begin to think about what’s outside the existing EHR box. These concepts are not mutually exclusive and you’ll see there’s overlap.
Let’s look at each of these innovative approaches.
EHR as Platform + Applications
Writing in the NEJM , Kenneth D. Mandl, M.D., M.P.H., and Isaac S. Kohane, M.D., Ph.D. describe a flexible way to develop EHRs.
An article in the New York Times summarized their thinking:
Instead of stimulating use of [pre-Internet EHR 1.0] software, they say, the government should be a rule-setting referee to encourage the development of an open software platform on which innovators could write electronic health record applications. As analogies, they point to other such software platforms — whether the Web or Apple ’s iPhone software, which the company has opened to outside developers.
Mandl and Kohane’s NEJM article lists examples of applications that could be developed:
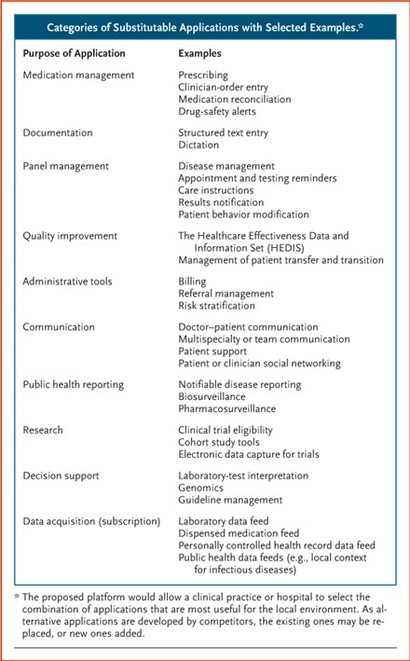
EHR as Clinical Groupware
David Kibbe describes his concept of Clinical Groupware . He asks “What would you call health care software that:
- Is Web-based and networkable, therefore highly scalable and inexpensive to purchase and use;
- Provides a ‘unified view’ of a patient from multiple sources of data and information;
- Is designed to be used interactively – by providers and patients alike – to coordinate care and create continuity;
- Offers evidence-based guidance and coaching, personalized by access to a person’s health data as it changes;
- Collects, for analysis and reporting, quality and performance measures as the routine by-product of its normal daily use;
- Aims to provide patients and their providers with a collaborative workflow platform for decision support; and
- Creates a care plan for each individual and then monitors the progress of each patient and provider in meeting the goals of that plan?”
EHR Integrated with PHR
What if Google Health and/or HealthVault added EHR functionality to their existing PHR functionality?
Read here for an example of what this might look like.
EHR as a “Publish-Discover” Search Engine
Vitaly Latush of Insimix wrote a whitepaper describing this approach. Here’s the basic idea:
(It’s) based on the “publish – discover” paradigm successfully used on the global scale to manage immense volumes of non-integrated information available through the Internet.
How can the complexities of large scale integration be avoided? Avoid integration. EHR is beyond the applicability limits of the integration approach. The solution is the “publish – discover” approach successfully used on the global scale to manage immense volumes of diverse information available through the Internet.
…not unlike your favorite internet search engine
EHR as Software-as-a-Service (SaaS)
Robert Rowley, MD, Chief Medical Officer of Practice Fusion describes his notion of EHR 2.0:
One can think of the traditional enterprise-type EHR systems as “EHR 1.0” and the newer generation of systems that are more SaaS-based as “EHR 2.0.” Not only are the newer generation of EHR systems less costly to implement (no need for local LAN system, no servers, no data backups, etc), they are less costly to maintain—local IT consultants may not even be needed if the system doesn’t require a full- fledged LAN with servers that require constant maintenance.
There’s one more innovative aspect of Practice Fusion’s software — it’s free, supported by ad revenues. According to Healthcare IT News , the company has over 13,000 users.
EHR + Disease Management Services = Care Coordination
I’ll add this option. Who says EHR functionality can only be provided by software — why not a blend of software and services? The HITECH requirements for “meaningful use” of EHRs include a specific reference to providing “care coordination”. Why not allow EHR vendors and/or physicians to meet this requirement by partnering with existing disease/care management companies or health plans?
DRT-Enabled EHR
HIT futurist Mark Anderson describes his thinking about Discrete Reportable Transcription (DRT):
A DRT-enabled EHR allows the physician to continue to dictate clinical notes for a specific period of time. The difference is that the DRT-enabled EHR populates discrete data via the transcription, reducing data entry time by 87%. In most cases, dictation is eliminated within the first nine months once the majority of the patients have been seen using a DRT-enabled EHR. Using multiple methods, a DRT-enabled EHR populates up to 95% of clinical data required for the creation of a clinical note, for orders, and for clinical outcome reporting.
What are other approaches to EHR 2.0?
This work is licensed under a Creative Commons Attribution-Share Alike 3.0 Unported License. Feel free to republish this post with attribution.
This is a good overview of the exciting possibilities. I agree that the government approach should be as a rule setting referee to define open standards and platforms rather than locking in existing proprietary protocols.
The key to making all of this work is interoperability standards. This should be the first priority. All of these applications will depend on having access to data in a standard format with well defined metadata. This would be the best service that the government could provide.
In an April 5th New York Times article (http://www.nytimes.com/2009/04/05/fashion/05iphone.html?_r=1&scp=2&sq=iphone&st=cse), developers were cashing in on Iphone apps (to the tune of $800k for one bright guy). It is obvious to me that the missing link in all our technology ideas is a simple one…what does the customer want? We continually focus on health plan needs (important) employer needs (very important), provider needs (very, very important) but miss out on the patient needs and wants and speculate on how they will want this and not want that. If we use the Platform + app model, then we allow for the market place to determine what will be effective and I suspect that Mandl and Kohane’s list will be a good starting point for for the first three groups but once patients start expressing what they want from an EHR/PHR, then it’ll be raining dogs
EHR 2.0: Thinking Outside the Cat Box (a great read from my friend vince k.): http://bit.ly/dcz45
EHR 2.0: Thinking Outside the Cat Box | e-CareManagement http://tinyurl.com/d32bd7
Added to EHRLinks.com
DELI EHR 2.0: Thinking Outside the Cat Box | e-CareManagement http://tinyurl.com/d32bd7
Excellent reflection!
It was as good a blog back then as it is today… what will EHR 2.0 look like? http://t.co/XkrXm7Z