Healthcare is fragmented…
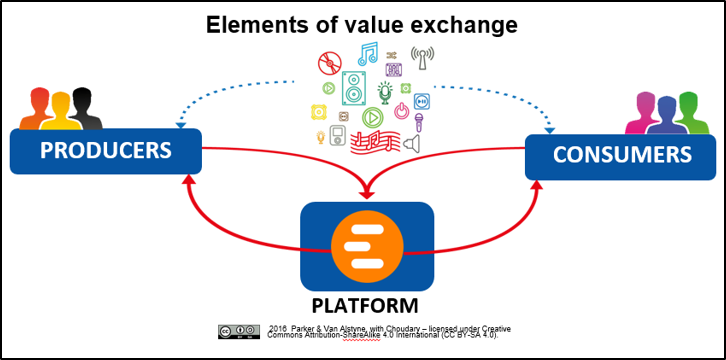
Platforms make connections and facilitate interactions…
Platforms are more than just technology.
Advising on
Healthcare strategy & business models for AI, platforms, digital health & ecosystems
Subscribe if you want to be notified of new blog posts. You will receive an email confirming your subscription.
The Healthcare Platform Blog formerly e-CareManagement Blog
Strategy & Business Models • Chronic Care • Technology • Policy
Your Company Has A Technology Platform…But Do You Have A Platform Business Model and Strategy?
Today in healthcare, platforms are understood mostly as technology. That’s not wrong, but it’s limiting and it misses a huge opportunity to adopt a platform business model.
In most other industries platforms are also understood as a business model and strategy. Outside of healthcare, there are 45+ books focusing on this topic.
This post is written for:
- 9,000+ early-stage digital health companies, most of which have a software and/or hardware technology platform as a centerpiece of their offering
- Healthcare incumbents — health systems, health plans, pharma, medical devices, etc. — that provide a digital platform as part of their external offering. For example, health systems that have an EHR platform, a patient portal, and/or a population health platform.
What Do Platforms Do?
Which Platform of Platforms (UDHP) is Right for your Health System? A Market Analysis
By Neil P. Jennings and Vince Kuraitis
In previous posts in this series, we have covered the definitions of Unified Digital Health platforms and whether “EHRs can become UDHPs.” In this follow-on post, we’ll talk through the requirements for success for a UDHP and which types of healthcare organizations are best suited for which types of UDHPs. This post will build on findings from the previous posts.
The Market Needs UDHPs: Key Takeaways from Previous Posts
Key Takeaway 1: The healthcare industry needs UDHPs to create a centralized, common architecture for healthcare organizations
Key Takeaway 2: The healthcare organizations leveraging UDHPs will achieve a myriad of benefits, from competitive advantages to clinical, financial, and operational gains
Key Takeaway 3: UDHPs are not all-or-nothing or mutually exclusive from EHRs. As we explored in our last post, EHRs could expand into UDHPs. These EHRs as UDHPs (or the relative platform of platforms) may be the optimal choice for some market segments. EHRs may also be accommodated into cloud-first UHDPs.
Key Takeaway 4 / Guiding Criterion: This post will focus on US regional and local health systems and outpatient groups of all sizes.
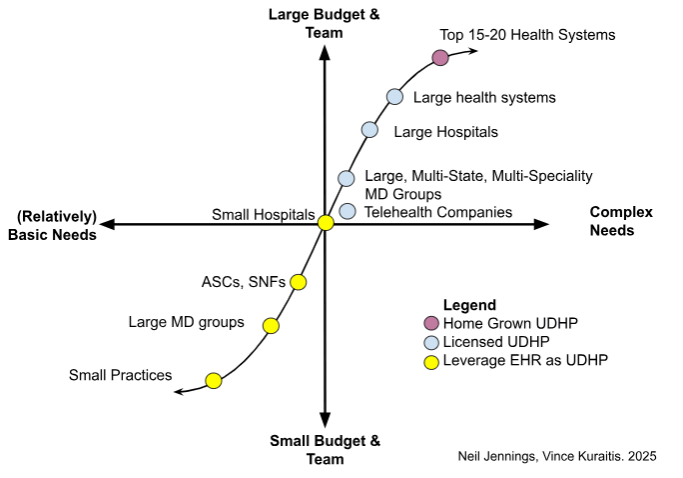
The Approach: Market -> Segments -> Options -> Fit
- For this post, we will start from the top-down market perspective, analyzing the overall market landscape.
- Once we have described the landscape, we will call out the key segments (organization types, sizes, and profiles) that we will be evaluating.
- At this point, we will approximate IT budgets and IT team sizes by organization type to determine capabilities of building as opposed to depending on partners and vendors.
- Then, we’ll review the constraints for implementation and ownership, outlining the drivers of UDHP fit.
- Next, we’ll break down the different ways UDHPs can be developed and maintained.
- Leveraging an EHR as UDHP
- License from UDHP vendor
- “Home grown” cloud-first solution
- Finally, we’ll crosswalk the segments and the optimal option for each segment, based on their specific needs and estimated IT and budgetary resources.
Can EHRs Expand to Become Health Systems’ “Platform of Platforms” (UDHPs)?
In a previous post in this series, we discussed healthcare’s migration toward Unified Digital Health Platforms (UDHPs) — a “platform of platforms.” Think of a UDHP as healthcare’s version of a Swiss Army knife: flexible, multi-functional, and (ideally) much better integrated than the drawer full of barely-used apps most health systems currently rely on.
We included a list of 20+ companies jockeying for UDHP dominance, including two familiar EHR (electronic health record) giants — Epic and Oracle. This raises the obvious question for today’s post:
Can EHRs level up into becoming UDHPs — becoming healthcare’s platform of platforms? Or are they trying to wear a superhero cape while tripping over their own cables?
We see good arguments pro and con, and like most things in healthcare “it’s complicated.” Some say EHRs are uniquely positioned to make the leap. Others believe the idea is like trying to teach your fax machine to run population health analytics.
Thus, we’ll lay out the arguments for differing points of view, and you can decide for yourself. Here’s an outline of today’s blog post:
- A Brief Recap: What are UDHPs?
- Thesis: EHRs Can Expand to Become UDHPs
- EHRs Currently Own the Customer Relationship
- Many Customers Have an “EHR-First” Preference for New Applications
- Epic and Oracle Health are Making Strong Movements Toward Becoming UDHPs
- Antithesis: EHRs Can NOT Become Effective EHRs
- EHRs Carry a Lot of Baggage
- Customers are Skeptical
- EHR Analytics Are NOT Optimized To Achieve Critical Health System Objectives
- EHR Switching Costs are Diminishing
- Cloud Native Platforms Accelerate Innovation and Performance
- It’s Not in EHR DNA to Become A Broad-Based Platform
- Synthesis and Conclusion
EXPERTISE IN PLATFORM STRATEGY & BUSINESS MODELS

Vince Kuraitis JD, MBA
Vince brings 30+ years’ healthcare executive and consulting experience across more than 150 organizations. Clients have included tech companies, hospitals, physician groups, IT, medical devices, pharma, health plans, disease management home health, and others. Vince received his graduate degrees at UCLA.

More than 12 years ago, Intel started a long journey to help build a consumer health ecosystem that would enable true patient empowerment and responsibility, care to the home and community, and personalized treatment using mobile devices and next generation diagnostics. With our many projects over the years, Vince has been far more than a just another consultant. He has become a confidant and collaborator—almost part of the Intel family—in helping to shape the wide range of investments we have made. From launching our early research on apps/wearables for independent living and chronic disease management…to initiating new conferences, standards organizations, and public policy initiatives to make way for personal health…to internal product and business plans we have developed, Vince has brought a careful, quiet, detailed wisdom that has helped us avoid the hype cycles of consumer health and to stay the course towards building an open, innovative ecosystem that is becoming more and more real by the day.
Eric Dishman, General Manager, Intel Health Strategy & Solutions Group