Subscribe if you want to be notified of new blog posts. You will receive an email confirming your subscription.
EHR

Can EHRs Expand to Become Health Systems’ “Platform of Platforms” (UDHPs)?
In a previous post in this series, we discussed healthcare’s migration toward Unified Digital Health Platforms (UDHPs) — a “platform of platforms.” Think of a UDHP as healthcare’s version of a Swiss Army knife: flexible, multi-functional, and (ideally) much better integrated than the drawer full of barely-used apps most health systems currently rely on.
We included a list of 20+ companies jockeying for UDHP dominance, including two familiar EHR (electronic health record) giants — Epic and Oracle. This raises the obvious question for today’s post:
Can EHRs level up into becoming UDHPs — becoming healthcare’s platform of platforms? Or are they trying to wear a superhero cape while tripping over their own cables?
We see good arguments pro and con, and like most things in healthcare “it’s complicated.” Some say EHRs are uniquely positioned to make the leap. Others believe the idea is like trying to teach your fax machine to run population health analytics.
Thus, we’ll lay out the arguments for differing points of view, and you can decide for yourself. Here’s an outline of today’s blog post:
- A Brief Recap: What are UDHPs?
- Thesis: EHRs Can Expand to Become UDHPs
- EHRs Currently Own the Customer Relationship
- Many Customers Have an “EHR-First” Preference for New Applications
- Epic and Oracle Health are Making Strong Movements Toward Becoming UDHPs
- Antithesis: EHRs Can NOT Become Effective EHRs
- EHRs Carry a Lot of Baggage
- Customers are Skeptical
- EHR Analytics Are NOT Optimized To Achieve Critical Health System Objectives
- EHR Switching Costs are Diminishing
- Cloud Native Platforms Accelerate Innovation and Performance
- It’s Not in EHR DNA to Become A Broad-Based Platform
- Synthesis and Conclusion

Webinar — Platform Shift: What is Beyond EHRs?
Our recent blog post “Platform Shift: From EHRs to UDHPs (Unified Digital Health Platforms)” has attracted a lot of attention. We’ll share highlights of the post and answer your questions in an upcoming webinar on Monday, April 28, at 1:00 PM Eastern time.
Jose Garcia will moderate a discussion among Girish Muralidharan, Jody Ranck, and me (Vince Kuraitis).
Register for the event by clicking on this link. Remember to use LinkedIn’s “Add to calendar” feature when you register. A recording will be available after the event.
Some of the 𝐭𝐨𝐩𝐢𝐜𝐬 𝐰𝐞’𝐥𝐥 𝐝𝐢𝐬𝐜𝐮𝐬𝐬:
- Why does healthcare need a “platform of platforms”?
- What are UDHPs (Unified Digital Health Platforms)?
- What are value propositions of UDHPs?
- What are examples of UDHPs? We’ll discuss two – 1) ServiceNow, a vendor case study, and 2) Mayo Clinic Platform, a healthcare provider case study
- What are some business and strategic implications of UDHPs? We’ll reference six.
Hope to see you there!
Platform Shift: From EHRs to UDHPs (Unified Digital Health Platforms)
by Vince Kuraitis, Girish Muralidharan*, and Jody Ranck*
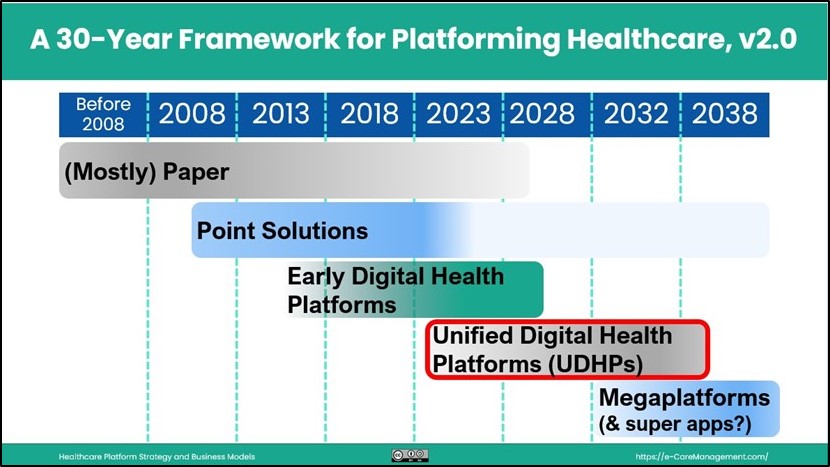
This essay is the next in the series entitled “Platforming Healthcare — the Long View”. The series presents a 30-Year Framework for Platforming Healthcare. An updated v2.0 of a graphic depicting this 30-Year Framework is shown above.
Today’s post will describe and discuss a potential successor to the EHR era — Unified Digital Health Platforms (UDHPs). Here’s an overview:
- Background and Environmental Trends
- Gartner’s Key Role in Characterizing the UDHP Movement
- UDHP Value Propositions
- Examples of UDHPs
- ServiceNow
- Mayo Clinic Platform
- Business and Strategic Implications of UDHPs
- APPENDIX: Additional Readings on UDHPs
This is a long post – about 4,000 words. So grab a cup of coffee and dig in.
*Disclosure: Girish Muralidharan previously worked at GE Healthcare, a UDHP vendor. Mayo Clinic Platform was a client of Ranck Consulting.
Background and Environmental Trends
Healthcare is fragmented. Data is not standardized and has existed in silos. Patients and clinicians have disjointed experiences. Payment structures create conflicting incentives.
Electronic Health Records (EHRs) were once touted as the key solution for transforming healthcare to a modern, digitally-enabled industry. Yet, they continue to frustrate clinicians with poor UI/UX and largely fulfill a primary role as a system of record to document claims submissions.
Recent technological and business trends have begun transforming healthcare into a more unified and integrated experience:
- HITECH (in the U.S.) drove the adoption of electronic health records across the industry
- Standards-compliant data models and APIs across various solutions are allowing third-party integrations to add new functionality
- Value-based care (VBC) and value-based payment (VBP) models incentivize improving quality rather than maximizing fee-for-service volumes
- AI’s emergence and adoption in healthcare fuels the need for more – and better – data and data liquidity.
- New competitors in healthcare (Big Tech, Big Retail, digital health ventures) compete based on improving patient experience, advancing VBC and VBP models, and integrated data and analytics
- Accessible cloud computing infrastructure is enabling a plethora of **-as-a-Service business models
Healthcare organizations want integrated solutions, not more point solutions. See the previous blog post in this series — “Beyond Awareness: Understanding the Magnitude of Point Solution Fatigue in Healthcare”.

Gartner’s Key Role in Characterizing the UDHP Movement
The trends and forces listed above open the door and create the need for a new category of enterprise software – Unified Digital Health Platforms (UDHPs).
A December 2022 Gartner Market Guide report characterized the long-term potential:
The DHP shift will emerge as the most cost-effective and technically efficient way to scale new digital capabilities within and across health ecosystems and will, over time, replace the dominant era of the monolithic electronic health record (EHR).

A 30-Year Framework for Platforming Healthcare
Healthcare has a reputation as being one of the most complex and fragmented industries. I’ll bet you’ve spent time pondering how we get ourselves out of this mess. This post is first in a series that takes a long-view perspective on platform adoption and evolution in healthcare. I’ll start by sharing Version 1.0 of “A 30-Year Framework for Platforming Healthcare” — see the graphic above.
A few weeks ago I was interviewed by Ruta Gabalina and Aiym Sarmanova of PPMI, a leading European research and policy analysis center. They are working on a study exploring the evolution of platforms in healthcare.
I shared my framework with them verbally, and now I say “thanks” for their creating a v1.0 graphic. It’s rough…gotta start somewhere 😐. I’ll greatly appreciate your reactions and suggestions for v2 and beyond.
Let’s take a look at the time frames listed in the graphic. The phases are not discrete — think of them as overlapping
Before 2008: (Mostly) Paper

The New Rules of Healthcare Platforms: APIs Enable the Platforming of Healthcare
by Vince Kuraitis, Brendan Keeler, and Jody Ranck
Recent regulations have mandated the use of HL7 FHIR APIs (application programming interfaces) to share health data. The regs apply to healthcare providers, payers, and technology developers who participate in federal programs. Many incumbent healthcare organizations are viewing these mandates as a compliance burden. That’s short-sighted. We recommend a more opportunistic POV.
APIs facilitate the sharing of health data across different devices and platforms. By adopting APIs, healthcare organizations can transform themselves from traditional service providers into powerful platforms that can connect patients, providers, and other stakeholders in new and innovative ways.
This blog post is the fourth in the series on The New Rules of Healthcare Platforms. In this essay, we explore the many benefits of API adoption for healthcare organizations and the key considerations that must be taken into account when implementing APIs:
- Healthcare’s Data Inflection Point
- APIs Enable Platform Business Models
- Barriers, Challenges, Reality Check

Today’s Patient Portals CAN NOT Work: An Inability to Capture Network Value
by Vince Kuraitis JD/MBA and Jody Ranck DrPH
Today’s patient portals are a mess. The catchphrase “Your mom has 7 portals for 7 providers” sums up patients’ frustrations and the resulting tepid utilization of portals. Today’s portals CAN NOT capture network value.
The first post in this series introduced the platform terminology of single-homing vs. multihoming. Patients strongly would prefer to have as few portals as possible — ideally one, i.e., a single “home”. However, patients are forced to subscribe to multiple homes since today’s portals are tethered to individual institutions or care providers.
In this post, we’ll introduce the platform terminology of stand-alone vs. network value. Today’s patient portals can provide some stand-alone value, but they provide minimal network value.
In the upcoming third post in the series, we’ll discuss “friction” in today’s portals. In the fourth post, we’ll consider some alternatives; while today’s portals CAN NOT work as configured, we’ll look at some options that could work.
Stand-Alone vs. Network Value
Value is created in different ways for different offerings. Some offerings provide stand-alone value; others provide value through networks and networked data and activities; some provide a combination of these.
Stand-alone value refers to the value provided by an offering that is independent of how the platform is used by others. Network value refers to value created through the activity and usage of others. Network value also refers to network effects or positive feedback loops created through the activities of others.
Let’s use your personal computer as an example to explain the difference between stand-alone vs. network value. Your PC has stand-alone value even when it is not connected to a network such as the internet.
Platform Terminology Explains Why Today’s Patient Portals CAN NOT Work
“…the patient portal, as currently architected, is a complete dead-end.”
—John Moore, Founder and Managing Partner, Chilmark Research
Patient portals have tremendous potential — but that potential has not been realized and *CAN NOT* be realized as portals are currently configured.
An understanding of platform business models and strategy explains why today’s patient portals are inherently suboptimal.
This essay is the first in an occasional series that will look at patient portals through the lenses of platform business models and strategy. Today’s post will introduce and explain platform terminology of multihoming and single homing. Future posts will look more deeply into “why” current patient portals can’t work and will propose options for portals that could work for patients.

Briefly Characterizing Today’s Patient Portals

Chilmark Podcast–Platform Thinking for Healthcare: A Discussion with Vince Kuraitis and Randy Williams
Dr. Randy Williams and I were interviewed by Jody Ranck of Chilmark Research. We discuss platform thinking for healthcare. Chilmark’s article contains a link to the podcast, a summary, and an “AI-generated” transcript.
Here are a few choice quotes from the podcast:
Vince: “EHRs are the poster child for a lack of platform thinking in health care”
Randy: “traditional business models really produce products and services, and they do that through taking the production side, integrating that and ultimately selling and delivering a product or a service to a customer….platform businesses really contrast with these traditional pipeline businesses by unlocking new sources of value both on the creation side of a transaction but also on the consumption side. Their function is really to facilitate matches or to consummate exchanges of goods and services, thereby creating value for all the parties.”

JAMIA Study Reports 22-68% Interoperability Across EHR Platforms: 7 Implications
by Vince Kuraitis, JD and Ian McNicoll, MD
A recent study of EHR interoperability found that 68% of data was “understood” when exchanged across different sites using the same vendor, but only 22% was “understood” when exchanged across different EHR vendors.
The study was published in the Journal of the American Medical Informatics Association (JAMIA). In this post, we will:
- Summarize the JAMIA study and its findings
- Interpret the findings
- Discuss possible solutions
- Describe seven implications
While we mostly agree on the study’s findings, we’ll offer some nuanced interpretations. Vince is a U.S. based healthcare consultant focusing on platform strategy and business models. Ian brings a European perspective – he is a former Scottish GP turned medical informatics expert.
Will Google Health Platformize the Electronic Health Record Market?
by Vince Kuraitis, Edward G. Anderson, and Geoffrey Parker
The COVID-19 pandemic has accelerated calls for the development of EHR 2.0 (electronic health record 2.0) – the next generation of EHRs with extended platform features and capabilities.
Who will answer this call? While existing EHR vendors have made modest efforts, the door is open for big tech companies and start-ups to develop functionality to envelop and disintermediate current EHRs. We highlight early efforts by Google Health Care Studio as having the potential to bring platform functionality to a sector of the healthcare industry known for resistance to change and innovation.
Read the full article in The Health Care Blog.